As vascular surgeon near me takes center stage, this opening passage beckons readers into a world crafted with good knowledge, ensuring a reading experience that is both absorbing and distinctly original. The unique skills and expertise required to become a successful vascular surgeon involve managing complex vascular conditions.
In this discussion, we will delve into the various aspects of vascular surgery, including the skills and expertise required to become a successful vascular surgeon, different types of vascular procedures, finding a trustworthy vascular surgeon, and the benefits of minimally invasive vascular procedures.
Vascular Surgeon Near Me: Understanding the Role of a Vascular Specialist in Modern Medicine
A vascular surgeon is a medical professional who specializes in treating conditions and diseases related to the vascular system, which includes blood vessels, arteries, and veins. Vascular specialists are highly trained experts who have the necessary skills and expertise to manage complex vascular conditions, making them a valuable asset to modern medicine.
To become a successful vascular surgeon, one must possess a unique combination of skills, knowledge, and expertise. These include advanced surgical skills, a deep understanding of vascular anatomy and physiology, as well as the ability to diagnose and treat complex vascular conditions. Vascular surgeons must also have excellent communication and interpersonal skills to effectively interact with patients, their families, and other healthcare professionals.
Types of Vascular Procedures Performed by Specialists
Vascular specialists perform a wide range of procedures to treat various vascular conditions, including both surgical and minimally invasive options. These procedures can be broadly categorized into two main types: open surgical procedures and endovascular procedures.
Open Surgical Procedures
Open surgical procedures involve making an incision in the skin to access the affected blood vessel. These procedures are often used for conditions such as aortic aneurysms, peripheral artery disease, and varicose veins. The surgeon will use a combination of traditional surgical techniques and advanced technologies, such as angioplasty and stenting, to repair the affected blood vessel.
Endovascular Procedures
Endovascular procedures, on the other hand, involve using a catheter to access the affected blood vessel through an incision in the skin or via a small opening in a peripheral artery. These procedures are often used for conditions such as carotid artery disease, renal artery stenosis, and venous reflux disease. The surgeon will use a combination of imaging technologies, such as fluoroscopy and ultrasound, to guide the catheter to the affected blood vessel.
Minimally Invasive Procedures
Minimally invasive procedures are a type of endovascular procedure that involves using a small incision and a specialized instrument to access the affected blood vessel. These procedures are often used for conditions such as varicose veins, spider veins, and peripheral artery disease. The surgeon will use a combination of advanced technologies, such as laser and radiofrequency ablation, to treat the affected blood vessel.
Specialized Techniques and Technologies
Vascular specialists use a wide range of specialized techniques and technologies to perform various vascular procedures. These include:
- Catheter-based interventions: These involve using a catheter to access the affected blood vessel and perform a procedure, such as angioplasty or stenting.
- Laser therapy: This involves using a laser to destroy or shrink the affected blood vessel.
- Radiofrequency ablation: This involves using heat generated by radiofrequency waves to destroy or shrink the affected blood vessel.
- Stent placement: This involves placing a stent, a small mesh tube, in the affected blood vessel to keep it open.
Benefits of Seeking Care from a Vascular Specialist
Seeking care from a vascular specialist can have numerous benefits, including:
- Early diagnosis and treatment of vascular conditions, reducing the risk of complications and improving patient outcomes.
- Advanced techniques and technologies, such as minimally invasive procedures and catheter-based interventions, to treat vascular conditions.
- Access to specialized expertise and training in vascular surgery, ensuring that patients receive the highest level of care.
- Improved patient outcomes, including reduced morbidity and mortality rates, and improved quality of life.
Choosing Between Different Types of Vascular Specialists
When dealing with vascular conditions, it’s essential to understand the role of different healthcare professionals who specialize in vascular care. Vascular surgeons, interventional radiologists, and other specialists play crucial roles in diagnosing and treating various vascular conditions. However, each specialist has their unique strengths and limitations, making it essential to choose the right expert for your specific needs.
Comparing Vascular Surgeons and Interventional Radiologists, Vascular surgeon near me
Vascular surgeons and interventional radiologists are two of the most common specialists dealing with vascular conditions. While they share some similarities, there are significant differences between their roles and areas of expertise.
– Vascular Surgeons:
A vascular surgeon is a medical doctor (MD) or a doctor of osteopathic medicine (DO) who specializes in surgical procedures to treat conditions affecting blood vessels, organs, and other tissues. Their expertise includes both surgical and non-surgical techniques to diagnose and treat various vascular conditions, such as peripheral artery disease (PAD), carotid artery disease, and aneurysms. Vascular surgeons often perform open surgery to repair or remove damaged tissue.
Vascular surgeons typically have more in-depth knowledge of surgical procedures and are trained to handle complex cases that may require surgical intervention. They work closely with other healthcare professionals, such as cardiologists and radiologists, to provide comprehensive care to their patients.
- Vascular surgeons perform open surgery to repair or remove damaged tissue.
- They have more in-depth knowledge of surgical procedures and are trained to handle complex cases.
- Vascular surgeons work closely with other healthcare professionals to provide comprehensive care.
– Interventional Radiologists:
An interventional radiologist is a medical doctor (MD) or a doctor of osteopathic medicine (DO) who specializes in image-guided, minimally invasive procedures to treat conditions affecting blood vessels and other organs. They use imaging technologies, such as X-rays, CT scans, or ultrasound, to guide their procedures and ensure precise treatment. Interventional radiologists often focus on treating vascular conditions without the need for open surgery.
Interventional radiologists typically have more expertise in imaging technologies and are trained to perform minimally invasive procedures. They work closely with other healthcare professionals to provide comprehensive care to their patients.
- Interventional radiologists use imaging technologies to guide their procedures.
- They are trained to perform minimally invasive procedures without the need for open surgery.
- Interventional radiologists work closely with other healthcare professionals to provide comprehensive care.
Other Specialized Healthcare Professionals
Besides vascular surgeons and interventional radiologists, other healthcare professionals also play crucial roles in treating vascular conditions. These include:
– Cardiothoracic Surgeons: They specialize in surgical procedures related to the heart and lungs. Some cardiothoracic surgeons may also perform vascular surgery, particularly when it involves the aortic arch or cardiac vessels.
– Neurosurgeons: They specialize in surgical procedures related to the brain, spine, and nervous system. Some neurosurgeons may also perform vascular surgery, particularly when it involves the cerebral vessels.
– Endovascular Specialists: They specialize in minimally invasive procedures to treat vascular conditions, using techniques such as balloon angioplasty and stent placement.
Choosing the right healthcare professional for your vascular needs depends on your specific condition and the best course of treatment. A thorough evaluation by a vascular specialist is crucial to determine the most appropriate treatment plan.
The Benefits of Minimally Invasive Vascular Procedures
Minimally invasive vascular procedures have revolutionized the field of vascular surgery, offering numerous benefits to patients. These modern techniques have made it possible for vascular specialists to perform complex operations with reduced scarring, faster recovery, and more comfort for the patients.
With the advancement in medical technology, vascular specialists can now treat a variety of vascular conditions, such as peripheral artery disease, varicose veins, and blocked arteries, without the need for lengthy hospital stays and extensive recovery periods. Minimally invasive vascular procedures have transformed the lives of patients, providing them with a better quality of life.
Reduced Scarring
One of the primary benefits of minimally invasive vascular procedures is reduced scarring. Traditional open surgery often results in visible scars, which can be unsightly and lead to self-consciousness. However, minimally invasive procedures use small incisions, often smaller than 1 cm, allowing for minimal scarring. The small incisions used for minimally invasive procedures are usually placed at the site of the procedure, making it difficult to notice any scarring.
Faster Recovery
Faster recovery is another significant advantage of minimally invasive vascular procedures. Since the incisions are small, patients experience less pain and swelling, allowing them to return to their normal activities quickly. Patients who undergo minimally invasive vascular procedures typically need less pain medication and may be able to resume their work or daily activities within a few days. This allows patients to get back to their normal routine sooner, minimizing the disruption to their lives.
Minimally Invasive Techniques
Minimally invasive vascular procedures use cutting-edge technology, such as vascular stents and catheters, to restore blood flow and alleviate symptoms. Vascular stents, made from metal or synthetic materials, are placed inside the affected blood vessel to keep it open and improve blood circulation. Catheters are thin, flexible tubes inserted into the blood vessel to inject medications, deliver clot-dissolving agents, or repair damaged areas.
By utilizing these modern technologies, vascular specialists can treat complex vascular conditions without the need for extensive surgery. The precision and accuracy of minimally invasive techniques ensure that the treatment is targeted and effective, reducing the risk of complications and promoting faster recovery.
Common Vascular Conditions Treated by Specialists
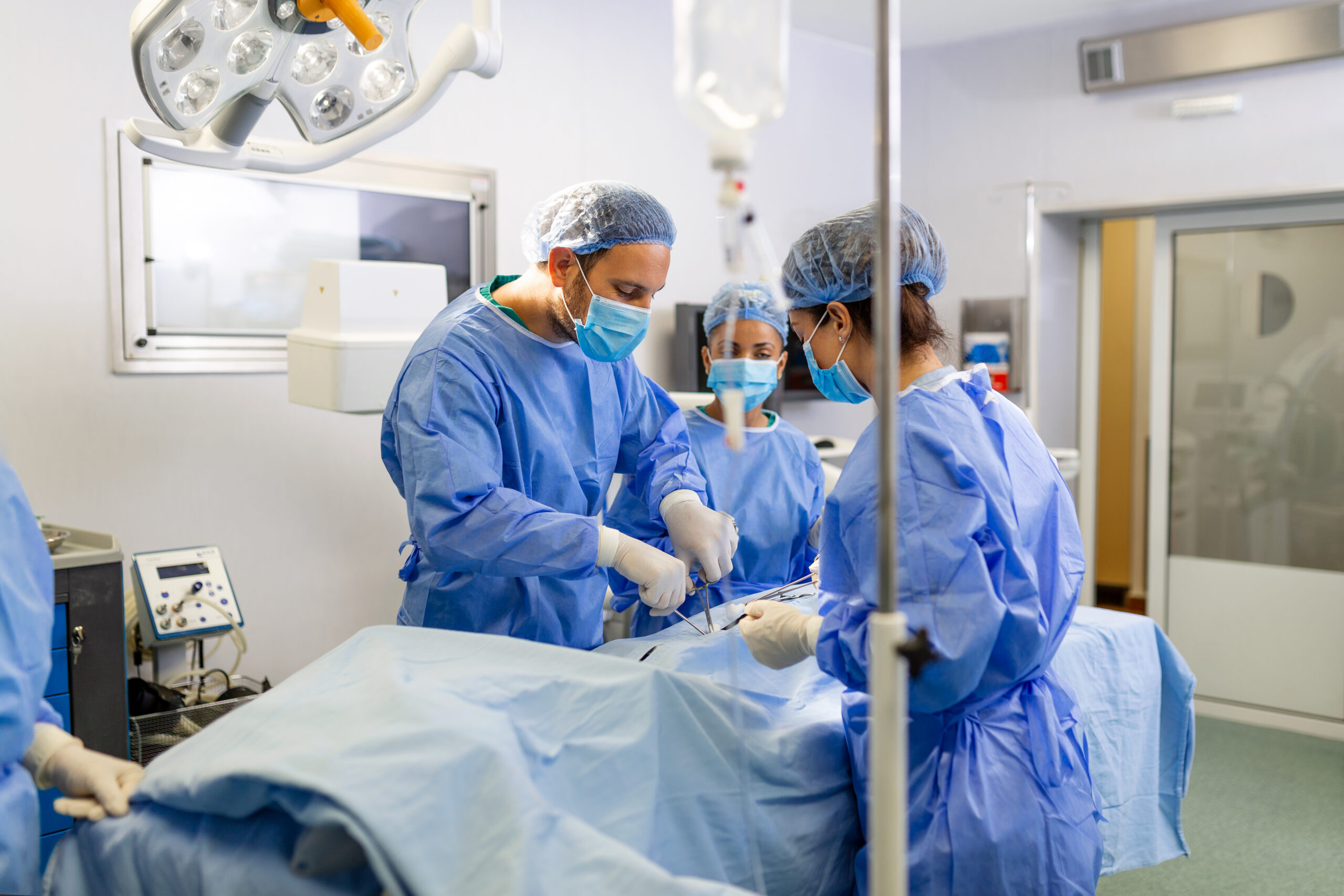
Vascular specialists treat a wide range of conditions that affect the blood vessels, including atherosclerosis, varicose veins, peripheral artery disease, aneurysms, and venous insufficiency. These conditions can be life-threatening if left untreated, and early diagnosis and treatment are crucial for preventing complications and improving outcomes.
Atherosclerosis
Atherosclerosis is a condition in which plaque builds up in the walls of the arteries, leading to narrowing and hardening of the arteries. This can cause a reduction in blood flow to the heart, brain, and other vital organs, increasing the risk of heart attacks, strokes, and other cardiovascular events. Atherosclerosis is a major cause of morbidity and mortality worldwide, affecting an estimated 100 million people globally.
Some of the key statistics about atherosclerosis include:
- It affects approximately 50% of adults over the age of 65.
- Men are more likely to develop atherosclerosis than women.
- In the United States alone, atherosclerosis is responsible for over 1 million deaths each year.
Peripheral Artery Disease (PAD)
PAD is a condition in which the arteries in the legs, arms, or other peripheral areas become narrowed or blocked, reducing blood flow to these areas. This can cause a range of symptoms, including pain or cramping in the legs, arms, or other areas, as well as weakness, fatigue, or aching in the affected area. PAD is a common condition, affecting an estimated 8.5 million adults in the United States.
Some of the key statistics about PAD include:
- Men are more likely to develop PAD than women.
- Smoking is a major risk factor for PAD.
- Hypertension and high cholesterol are also significant risk factors.
- PAD is associated with an increased risk of heart attacks and strokes.
Aneurysms
An aneurysm is a bulging or swelling of a blood vessel, which can rupture and cause internal bleeding. Aneurysms are a serious condition that requires prompt medical attention. There are several types of aneurysms, including aortic aneurysms, which occur in the aorta, and peripheral aneurysms, which occur in smaller blood vessels.
Some of the key statistics about aneurysms include:
- Aneurysms affect over 1.2 million people in the United States each year.
- Men are more likely to develop aneurysms than women.
- Smoking is a major risk factor for aneurysms.
- High blood pressure and high cholesterol are also significant risk factors.
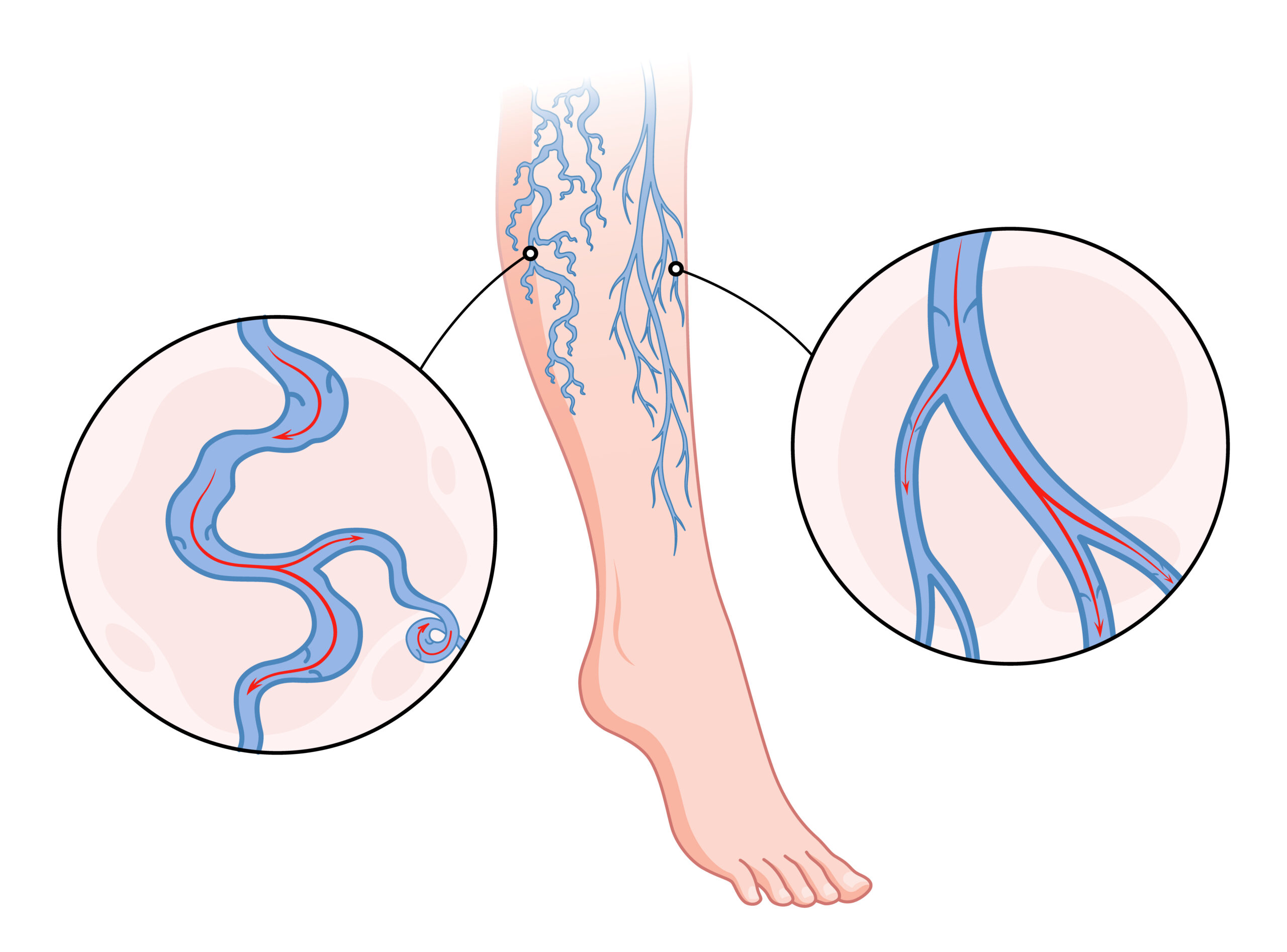
Varicose Veins
Varicose veins are a condition in which the veins in the legs or other areas become enlarged and twisted, causing a range of symptoms including pain, swelling, and discoloration. Varicose veins are a common condition, affecting an estimated 24% of adults in the United States.
Some of the key statistics about varicose veins include:
- Women are more likely to develop varicose veins than men.
- Obesity and pregnancy are also significant risk factors.
- Varicose veins are associated with an increased risk of venous thromboembolism.
- Treatment options for varicose veins include surgery, sclerotherapy, and endovenous ablation.
Venous Insufficiency
Venous insufficiency is a condition in which the veins in the legs or other areas become unable to return blood to the heart properly, leading to a range of symptoms including swelling, pain, and fatigue. Venous insufficiency is a common condition, affecting an estimated 40% of adults in the United States.
Some of the key statistics about venous insufficiency include:
- Women are more likely to develop venous insufficiency than men.
- Pregnancy and obesity are also significant risk factors.
- Venous insufficiency is associated with an increased risk of venous thromboembolism.
- Treatment options for venous insufficiency include compression stockings, elevating the affected area, and surgery.
Advanced Vascular Surgery Techniques
Vascular surgery has evolved significantly over the years, with the introduction of innovative techniques and technologies that have revolutionized the way vascular specialists approach complex cases. Advanced vascular surgery techniques, such as endovascular repair, carotid artery stenting, and vascular bypass grafts, have become essential tools in the management of various vascular diseases.
These procedures offer significant benefits over traditional open surgery, including reduced recovery time, less blood loss, and reduced risk of complications. In addition, advanced vascular surgery techniques allow for the treatment of complex cases that may not have been treatable with traditional methods. Advanced vascular surgery techniques are used to repair and replace damaged or diseased blood vessels, restore blood flow to tissues, and prevent further vascular complications.
Endovascular Repair
Endovascular repair is a minimally invasive procedure used to treat aortic aneurysms and other vascular diseases. The procedure involves the insertion of a catheter through a small incision in the groin, which is then guided to the affected blood vessel. A stent or graft is deployed through the catheter, which expands to conform to the shape of the blood vessel. This prevents further damage to the vessel and restores blood flow to the affected area.
Benefits of Endovascular Repair
- Minimally invasive procedure reduces risk of complications and promotes faster recovery
- No need for open surgery, which reduces risk of infections and blood loss
- Allows for treatment of complex cases that may not have been treatable with traditional methods
- Restores blood flow to tissues, improving overall health outcomes
Carotid Artery Stenting
Carotid artery stenting is a procedure used to treat blocked or narrowed carotid arteries, which supply blood to the brain. The procedure involves the insertion of a stent through a small incision in the groin, which is then guided to the affected carotid artery. The stent is deployed to widen the narrowed area, restoring blood flow to the brain.
Benefits of Carotid Artery Stenting
- Minimally invasive procedure reduces risk of complications and promotes faster recovery
- No need for open surgery, which reduces risk of infections and blood loss
- Restores blood flow to the brain, reducing risk of stroke and other cerebrovascular events
- Can be performed on patients who are not good candidates for carotid endarterectomy
Vascular Bypass Grafts
Vascular bypass grafts are used to treat blocked or narrowed blood vessels, which can lead to poor circulation in the legs, feet, and other areas. The procedure involves the insertion of a graft, usually made of synthetic or biologic material, through a small incision in the groin or arm. The graft is then connected to the affected blood vessel, providing a new pathway for blood to flow.
Benefits of Vascular Bypass Grafts
- Restores blood flow to tissues, improving overall health outcomes
- Can be used to treat a variety of vascular diseases, including peripheral artery disease
- Minimally invasive procedure reduces risk of complications and promotes faster recovery
- No need for open surgery, which reduces risk of infections and blood loss
Preoperative Preparation Required for Vascular Surgery
Preoperative preparation for vascular surgery involves a thorough assessment of the patient’s overall health, including their medical history, medications, and lifestyle habits. The goal of preoperative preparation is to identify any potential risks or complications that may arise during or after surgery, and to develop a plan to manage these risks.
Preoperative Preparation Steps
- Risk assessments: Patients undergo a thorough risk assessment to identify any potential risks or complications that may arise during or after surgery
- Medication management: Patients are advised to stop taking certain medications, such as blood thinners, before surgery
- Lifestyle adjustments: Patients are advised to make lifestyle adjustments, such as quitting smoking and following a healthy diet, to reduce their risk of complications
- Patient education: Patients are educated on the risks and benefits of vascular surgery, as well as what to expect during and after surgery
By understanding the preoperative preparation required for vascular surgery, patients can feel more confident and prepared for their procedure, and can work collaboratively with their vascular specialist to develop a plan to manage any potential risks or complications.
Outcome Summary
In conclusion, finding a trustworthy vascular surgeon is crucial for receiving proper treatment for vascular conditions. By understanding the unique skills and expertise required to become a successful vascular surgeon, patients can make informed decisions about their treatment options. Additionally, patients should be aware of the different types of vascular procedures and the benefits of minimally invasive techniques.
Question Bank
What is the difference between a vascular surgeon and an interventional radiologist?
A vascular surgeon is a medical doctor who specializes in surgical procedures to repair or remove diseased or damaged blood vessels, while an interventional radiologist is a physician who uses imaging guidance to perform minimally invasive procedures to diagnose and treat vascular conditions.
What are the benefits of minimally invasive vascular procedures?
Minimally invasive vascular procedures offer several benefits, including reduced pain, shorter hospital stays, and quicker return to normal activities. These procedures also reduce the risk of complications and scarring.
How do I find a trustworthy vascular surgeon in my area?
To find a trustworthy vascular surgeon, research their credentials, including education, certifications, and professional affiliations. Check online reviews and patient satisfaction surveys to ensure they have a good bedside manner and communication skills.
What are some common vascular conditions treated by specialists?
Common vascular conditions treated by specialists include atherosclerosis, varicose veins, peripheral artery disease, aneurysms, and venous insufficiency.