As cornea transplant doctors near me takes center stage, this opening passage beckons readers into a world crafted with good knowledge, ensuring a reading experience that is both absorbing and distinctly original. The process of corneal transplantation is a complex procedure that requires expertise and precision, making it crucial to find the right doctor to guide you through the process.
Cornea transplants are a type of surgery that replaces a damaged or diseased cornea with a healthy one from a donor. The procedure involves several steps, including evaluation, surgery, and post-operative care. There are also different types of corneal transplants, such as penetrating keratoplasty and endothelial keratoplasty, each with its own unique benefits and risks.
What Are Cornea Transplants and How Do They Work?
Corneal transplantation, also known as corneal grafting, is a medical procedure where a damaged or diseased cornea is replaced with a healthy donor cornea. This complex process involves a delicate balance of surgical techniques, immunosuppressive medications, and post-operative care to ensure the best possible outcome for the recipient.
The cornea, the clear, dome-shaped surface at the front of the eye, is responsible for refracting light and allowing it to enter the eye. In some cases, the cornea may become damaged or diseased due to injury, infection, or genetic disorders. Corneal transplantation is a life-changing procedure that restores vision and improves quality of life for those affected.
There are several types of corneal transplants, each with its own unique characteristics and indications:
Types of Corneal Transplants
-
Penetration Keratoplasty (PK)
: In this procedure, a shallow layer of the damaged cornea is removed and replaced with donor tissue.
-
Endothelial Keratoplasty (EK)
: This involves replacing only the innermost layer of the cornea, where the endothelial cells reside.
-
Deep Anterior Lamellar Keratoplasty (DALK)
: This procedure involves removing the front portion of the cornea, including the epithelium and Bowman’s layer, and replacing it with donor tissue.
The choice of transplant type depends on the extent and location of the corneal damage, as well as the patient’s overall eye health.
Surgical Techniques
Corneal transplantation requires a precise and delicate approach to ensure the best possible outcome. The donor cornea is typically obtained from a eye bank and is matched with the recipient for blood type, tissue type, and other criteria. The surgical procedure involves:
-
Local or general anesthesia to ensure patient comfort and relaxation
-
Creation of a corneal incision, typically in the form of a partial thickness incision or a linear incision
-
Removal of the damaged or diseased cornea and any surrounding tissue
-
Implantation of the donor cornea, either with or without the endothelial layer (depending on the type of transplant)
-
Securing of the donor graft with sutures and application of topical antibiotics to promote healing
The entire procedure typically takes several hours to complete and is performed in a sterile environment to minimize the risk of infection.
The donor cornea is usually obtained from an eye bank, which obtains and processes corneas from donors who have consented to donating their corneas after deceased. The donor cornea is then stored in a specialized medium and shipped to the recipient’s location, where it is prepared for transplantation.
Corneal transplantation is a complex procedure that requires meticulous attention to detail and a deep understanding of the underlying anatomy and pathology. By using the latest surgical techniques and advancements in immunosuppressive medications, corneal transplantation can restore vision and improve the quality of life for those affected by corneal damage or disease.
Preparing for a Cornea Transplant: A Patient’s Journey
As you prepare for a cornea transplant, it’s essential to understand the steps involved in this life-changing process. Your journey will begin with a thorough evaluation and testing to determine the best course of action for your unique situation.
Pre-Operative Preparations
Preparations for a cornea transplant typically begin several weeks or even months before the actual surgery. This allows your medical team to monitor your condition closely and ensure you’re in the best possible state for the transplant. To minimize any potential risks, you may be prescribed medications to prevent rejection or promote healing. Medications may include immunosuppressants, antibiotics, and anti-inflammatories.
Your eye care professional may also instruct you to use eye drops to reduce swelling and promote healing. These eye drops may contain ingredients such as steroid, non-steroidal, and vasoconstrictors to alleviate discomfort and inflammation. Additionally, you may be instructed to avoid certain activities or medications that could interfere with the success of the transplant.
Pre-Surgery Precautions, Cornea transplant doctors near me
In the days leading up to the transplant, it’s essential to follow your medical team’s instructions carefully. This may include:
- Eating a healthy and balanced diet to maintain your overall health
- Avoiding heavy lifting, bending, or strenuous activities
- Staying hydrated by drinking plenty of water and other fluids
- Managing any underlying medical conditions, such as diabetes or hypertension
It’s also crucial to understand that a cornea transplant is a serious surgical procedure that requires significant recovery time. Your medical team will provide detailed instructions on how to prepare for and recover from the transplant.
Post-Operative Care and Recovery
After the transplant, your medical team will closely monitor your progress and provide guidance on post-operative care. This may include:
- Resting your eyes and avoiding strenuous activities for several weeks
- Applying eye drops as instructed by your eye care professional to promote healing and reduce inflammation
- Attending follow-up appointments to ensure proper healing and address any concerns or complications
- Following a healthy diet and staying hydrated to support your body’s recovery
While every individual’s experience with a cornea transplant is unique, it’s essential to be aware of potential complications and risks. These may include:
- Rejection of the transplanted cornea
- Infection or inflammation of the eye
- Visual disturbance or loss
- Prolonged recovery time or complications during the healing process
It’s essential to carefully follow your medical team’s instructions and attend follow-up appointments to minimize the risk of complications and ensure a successful recovery.
It’s essential to understand that a cornea transplant is a complex and serious surgical procedure that requires dedication, patience, and a commitment to follow precise instructions.
4. Finding the Right Cornea Transplant Doctor Near Me
Your search for the right cornea transplant doctor near you is a crucial step in the journey towards restoring your vision. In this section, we will delve into the key factors to consider when evaluating a corneal surgeon or eye specialist, as well as the pros and cons of seeking treatment from a local hospital versus a specialized eye clinic.
Credentials and Qualifications of a Corneal Surgeon or Eye Specialist
A highly skilled and experienced cornea transplant surgeon or eye specialist is a vital component in ensuring a successful surgical outcome. When searching for a cornea transplant doctor, look for the following credentials and qualifications:
- Board Certification: Ensure that the corneal surgeon or eye specialist is board certified by a reputable professional organization, such as the American Board of Ophthalmology (ABO) or the American Osteopathic Board of Ophthalmology and Otolaryngology (AOBOO). This certification indicates that the doctor has completed the necessary training and has demonstrated expertise in the field.
- Subspecialty Training: Corneal surgery is a subspecialty of ophthalmology, so it’s essential to find a doctor with advanced training in corneal surgery, such as a fellowship in corneal surgery.
- Experience: Look for a doctor with extensive experience in performing cornea transplants, preferably with a large volume of cases. This will give you the best chance of a successful outcome.
- Professional Affiliations: Check if the doctor is a member of professional organizations, such as the Cornea Society or the American Academy of Ophthalmology (AAO), which demonstrate a commitment to staying up-to-date with the latest advancements in corneal surgery.
- Peer-Reviewed Publications: Check if the doctor has published research papers in reputable peer-reviewed journals. This indicates their expertise and contributions to the field.
By considering these credentials and qualifications, you can increase your chances of finding a skilled and experienced cornea transplant surgeon or eye specialist to perform your surgery.
Local Hospital Versus Specialized Eye Clinic
When evaluating treatment options, you may be faced with the decision of whether to seek treatment from a local hospital or a specialized eye clinic. While both options have their benefits, there are some key differences to consider:
Pros of a Local Hospital:
Local hospitals often have a wide range of medical specialties and subspecialties available, including ophthalmology. This can be beneficial if you need additional medical care or have pre-existing medical conditions that need to be addressed before your surgery. Additionally, local hospitals often have a network of specialists that can be called upon in case of complications or emergency situations.
Cons of a Local Hospital:
Local hospitals may not have specialized equipment or expertise in corneal surgery, which can impact the quality of care you receive. Additionally, the costs of care may be higher due to the overhead of running a large hospital.
Pros of a Specialized Eye Clinic:
Specialized eye clinics have experienced cornea transplant surgeons or eye specialists who have dedicated their practice to treating eye-related conditions. These clinics often have state-of-the-art equipment and a team of healthcare professionals dedicated to providing expert care. Additionally, the costs of care may be lower due to the specialized focus of the clinic.
Cons of a Specialized Eye Clinic:
While specialized eye clinics can offer high-quality care, they may not have the same level of comprehensive medical services available. Additionally, the cost of care may be higher than at a local hospital, depending on the specific clinic and services offered.
By carefully weighing the pros and cons of each option, you can make an informed decision about where to receive your cornea transplant care.
What to Ask Your Ophthalmologist Before the Cornea Transplant Surgery
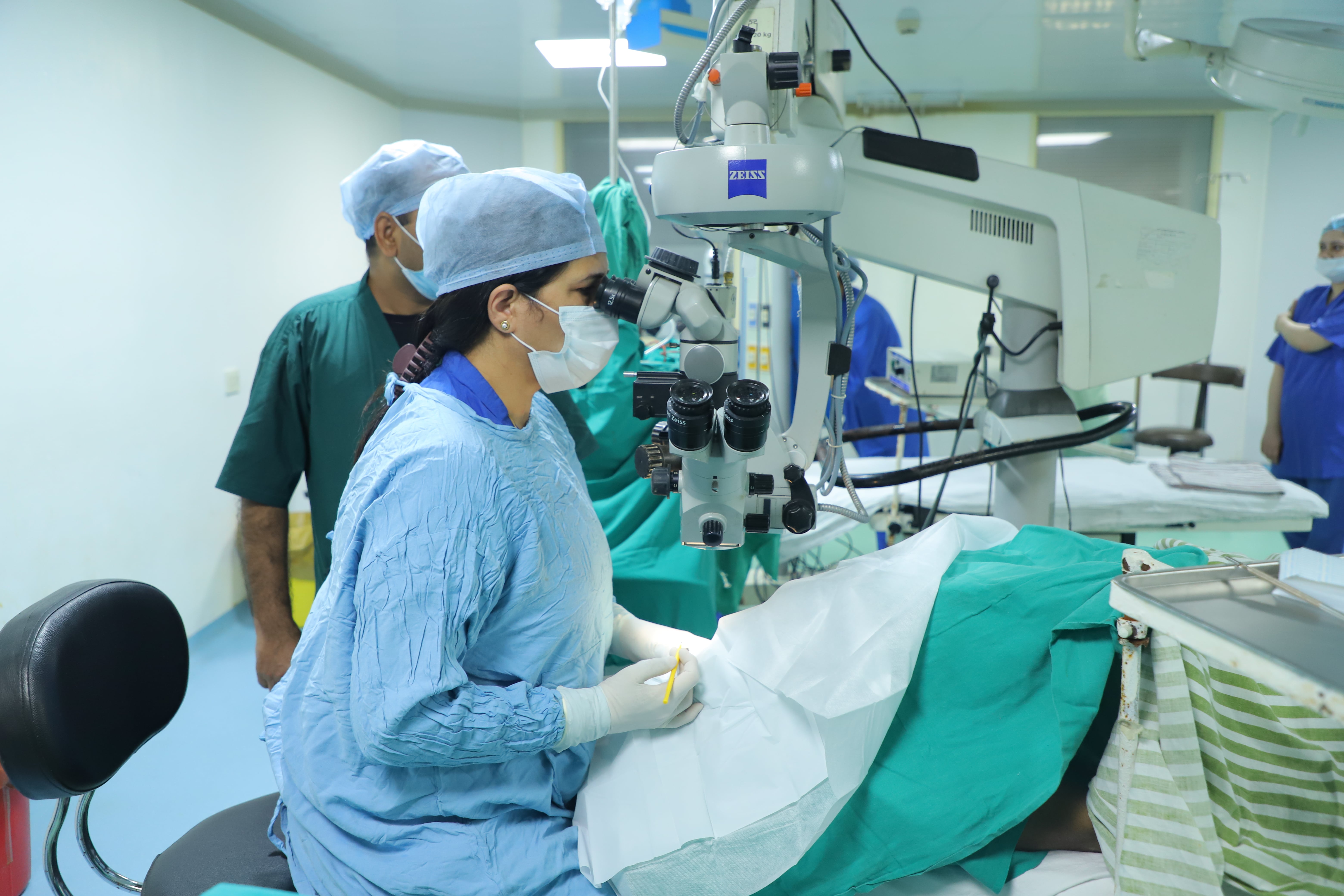
As the day of your cornea transplant surgery approaches, it is essential to prepare yourself with the right questions to ask your ophthalmologist. This will not only ease your anxiety but also ensure that you are fully aware of the surgical procedure and its outcomes. Your ophthalmologist is your guide throughout this journey, and their expertise and experience are crucial to a successful outcome.
To make the most of this opportunity, it is vital to ask the right questions and understand the answers. This will not only provide peace of mind but also help you make informed decisions about your care.
Understanding the Surgical Process
Understanding the cornea transplant surgery process is crucial to your recovery. Your ophthalmologist should explain the procedure in detail, including the type of transplant, the surgical technique, and the expected outcomes.
- What type of cornea transplant will I undergo (e.g., penetrating keratoplasty, endothelial keratoplasty)?
- What are the risks and complications associated with the surgery?
They should discuss the specifics of the procedure, including the type of cornea transplant, the surgical technique, and any specialized equipment used. Additionally, they should explain the expected outcomes, including the likelihood of visual improvement, potential complications, and post-operative care requirements.
They should discuss any potential risks and complications associated with the surgery, such as infection, graft rejection, or vision loss. Understanding these risks will help you prepare for the surgery and its potential outcomes.
Preparation and Post-Operative Care
To ensure a smooth recovery, your ophthalmologist should provide clear guidance on preparation and post-operative care. This includes instructions on medication, wound care, and follow-up appointments.
- What medications will I need to take before and after surgery?
- What are the post-operative care instructions, including wound care and follow-up appointments?
- When can I expect to see improvements in my vision?
- Are there any long-term implications or potential complications?
- Do they take the time to address your questions and concerns?
- Are they able to provide emotional support and reassurance?
- Do they explain the risks and benefits in a clear and transparent manner?
- Attend regular follow-up appointments with your ophthalmologist to monitor the healing process and address any concerns.
- Use protective eye gear, such as goggles or protective shields, when showering, bathing, or engaging in activities that may cause water to splash into your eyes.
- Avoid strenuous activities, such as heavy lifting or bending, which may cause increased pressure on the cornea.
- Rest your eyes frequently and avoid rubbing or touching the operated eye.
- Use artificial tears or lubricating drops as directed by your ophthalmologist to maintain eye moisture and comfort.
- Avoid exposure to dust, wind, or other environmental factors that may irritate the cornea.
- Take medications as prescribed by your ophthalmologist to prevent infection and promote healing.
- Wear sunglasses with UV protection to shield your eyes from the sun’s rays.
- Use pain management medications, such as acetaminophen or ibuprofen, as directed by your ophthalmologist to alleviate discomfort.
- Apply cold compresses or ice packs to the closed eye to reduce swelling and pain.
- Avoid rubbing or touching the operated eye to prevent irritation and discomfort.
- Use lubricating drops or ointments as directed by your ophthalmologist to maintain eye moisture and comfort.
- Rest your eyes frequently and avoid straining or overexertion, which may exacerbate eye pain and discomfort.
- Consider using a warm compress or a warm washcloth to soothe the eyelid and promote healing.
They should discuss any medications that you will need to take before and after surgery, including any prescription medications, over-the-counter medications, or supplements. Understanding your medication regimen will help you manage your recovery.
They should provide clear instructions on wound care, including how to protect the eye, manage pain, and maintain good hygiene. Additionally, they should schedule follow-up appointments to monitor your progress and address any concerns.
Recovery and Visual Outcomes
Your ophthalmologist should provide an overview of your recovery and the expected visual outcomes. This includes information on when you can expect to see improvements in your vision and any long-term implications.
They should discuss the timeline for expected improvements in vision, including any initial recovery period and the possibility of gradual improvements over the next few months.
They should discuss any long-term implications or potential complications associated with the surgery, including the risk of graft rejection or vision loss.
Evaluating Your Ophthalmologist’s Bedside Manner and Communication Skills
Your ophthalmologist’s bedside manner and communication skills are essential to your overall care and satisfaction. You should evaluate their ability to listen, explain complex information, and provide reassurance.
They should be able to take the time to address your questions and concerns, providing clear and concise explanations of complex information.
They should be able to provide emotional support and reassurance, addressing any anxieties or fears you may have about the surgery.
They should be able to explain the risks and benefits in a clear and transparent manner, avoiding technical jargon and complicated terms.
After the Transplant: A Journey of Healing and Rehabilitation: Cornea Transplant Doctors Near Me
The road to recovery after a cornea transplant surgery can be a challenging but ultimately rewarding experience. It requires patience, dedication, and a thorough understanding of the healing process. As you embark on this journey, it’s essential to take necessary precautions to reduce the risk of complications and manage eye pain and discomfort effectively.
Precautions to Take During the Recovery Period
During the recovery period, which typically lasts several weeks, it’s crucial to take certain precautions to ensure smooth healing and minimize the risk of complications. Some of these precautions include:
These precautions will help you navigate the recovery period and minimize the risk of complications, such as infection, scarring, or rejection of the transplanted cornea.
Managing Eye Pain and Discomfort
Eye pain and discomfort are common symptoms after a cornea transplant surgery. However, there are strategies to help manage these symptoms and promote a smooth recovery.
By following these strategies, you can effectively manage eye pain and discomfort and promote a smooth recovery after your cornea transplant surgery.
Final Summary
Corneal transplantation is a life-changing procedure that can restore vision and improve the quality of life for individuals with corneal diseases. Finding the right cornea transplant doctor near me requires careful research and consideration of several factors, including credentials, experience, and patient reviews. By taking the time to research and prepare, individuals can ensure the best possible outcome for their corneal transplant surgery.
Quick FAQs
What are the common causes of corneal disease?
Corneal disease can be caused by various factors, including infections, injuries, aging, and genetic disorders. Some common causes of corneal disease include keratoconus, corneal ulcers, and Fuchs’ endothelial dystrophy.
How long does it take to recover from corneal transplant surgery?
The recovery time for corneal transplant surgery can vary depending on the individual and the type of surgery performed. Generally, patients can expect to experience some discomfort, blurring of vision, and sensitivity to light for several weeks after surgery.
Can I get a corneal transplant if I have a pre-existing medical condition?
Patients with pre-existing medical conditions, such as diabetes or hypertension, may be eligible for corneal transplant surgery. However, it’s essential to discuss your medical history with your doctor to determine the risks and benefits of the surgery.
How long do corneal transplants last?
Corneal transplants can last for decades with proper care and maintenance. However, the lifespan of the transplant can depend on various factors, including the type of surgery, the health of the patient, and the presence of any underlying medical conditions.