Electroconvulsive therapy near me sets the stage for this enthralling narrative, offering readers a glimpse into a story that is rich in detail and brimming with originality from the outset. This fascinating tale of human resilience and determination to seek aid from a complex and often misunderstood treatment option will captivate you and leave you eager to learn more.
This is a journey where the lines between science and art blur, where a treatment once shrouded in mystery and fear steps into the spotlight, and where the voices of those who have benefited from it share their stories. So, join us as we delve into the world of electroconvulsive therapy and unravel its intricacies to reveal the truth behind this powerful medical treatment.
Understanding the Procedure and Mechanism of Electroconvulsive Therapy
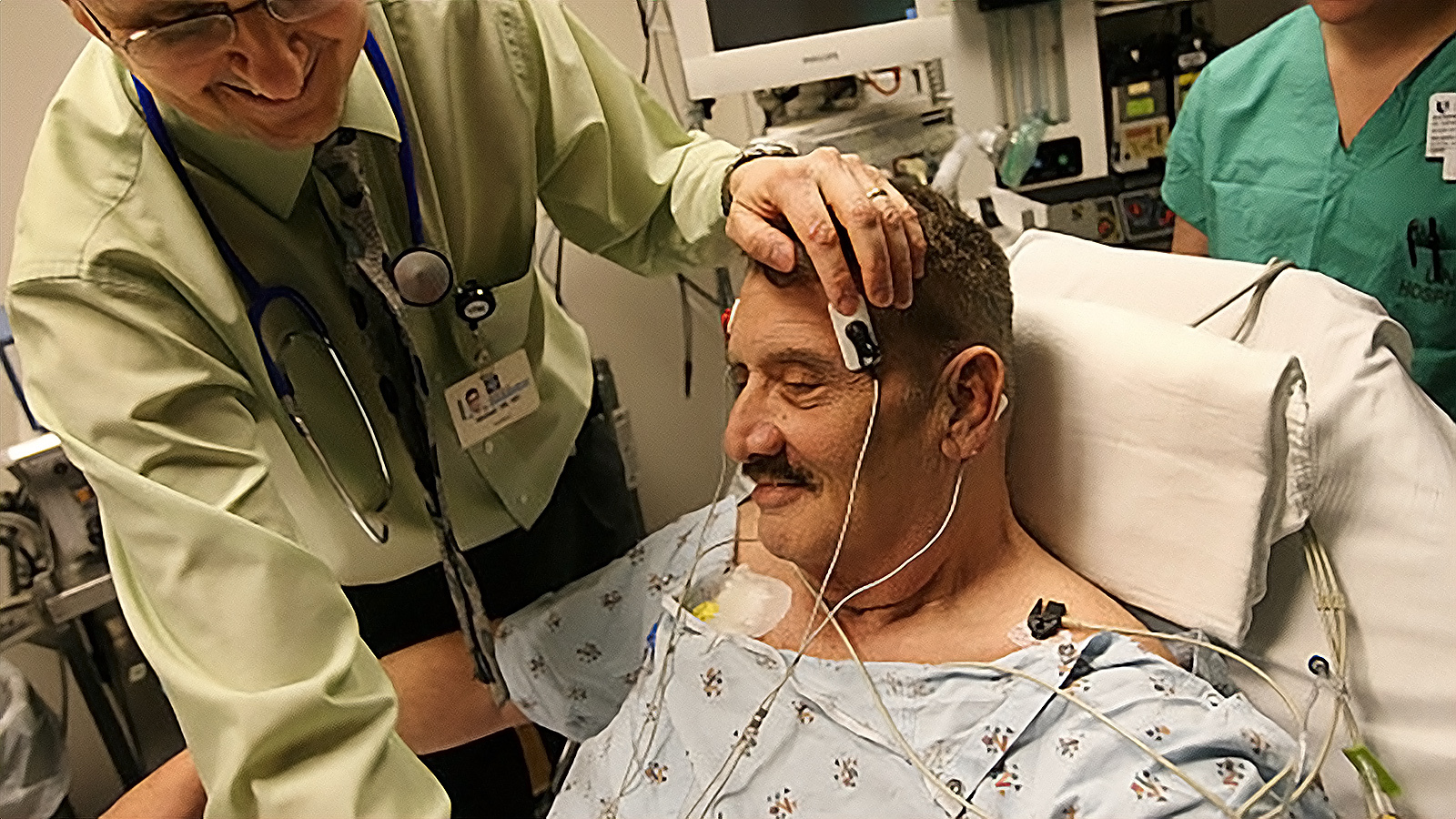
Electroconvulsive therapy (ECT) is a treatment used to help individuals with severe mental illnesses, such as depression, bipolar disorder, and schizophrenia. The procedure involves the use of electrical impulses to stimulate the brain, causing a controlled seizure. Despite its effectiveness, many people remain wary of ECT due to misunderstandings about the procedure. This discussion aims to provide a detailed understanding of the technical aspects of ECT, including the equipment used, the administration process, and potential side effects.
The equipment used in ECT includes a device specifically designed for the purpose, such as a Thymatron device, and electroencephalographic (EEG) electrodes placed on the patient’s scalp. The administration process typically involves the patient being given general anesthesia and muscle relaxants to prevent pain and discomfort during the procedure. The anesthesiologist ensures the patient’s safety and comfort throughout the process.
The Role of General Anesthesia and Muscle Relaxants during ECT
General anesthesia is necessary to prevent pain and discomfort during the procedure. Muscle relaxants are also administered to prevent muscle contractions, which can be triggered by the electrical impulses. This combination of medications ensures that the patient remains safe and comfortable throughout the procedure.
- General anesthesia is administered to induce unconsciousness and prevent pain during the procedure.
- Muscle relaxants are given to prevent muscle contractions, which can be triggered by the electrical impulses.
- Electroencephalographic (EEG) electrodes are placed on the patient’s scalp to monitor the electrical activity in the brain.
Comparing and Contrasting ECT with Other Forms of Psychiatric Treatment, Electroconvulsive therapy near me
ECT is often compared and contrasted with other forms of psychiatric treatment, such as medication, psychotherapy, and cognitive-behavioral therapy. The following table highlights the main differences:
| Treatment | Effectiveness | Side Effects | Recovery Time |
|---|---|---|---|
| ECT | Highly effective in severe cases of mental illness | Potential side effects include memory loss and confusion | Quick recovery, with most patients returning to normal within hours |
| Medication | Effective in mild to moderate cases of mental illness | Potential side effects include dependence and withdrawal symptoms | Prolonged recovery time, depending on the medication and individual response |
| Psychotherapy | Effective in mild to moderate cases of mental illness | Potential side effects include emotional exhaustion and burnout for therapists | Prolonged recovery time, depending on the individual response and therapy type |
| Cognitive-Behavioral Therapy | Effective in mild to moderate cases of mental illness | Potential side effects include emotional exhaustion and burnout for therapists | Prolonged recovery time, depending on the individual response and therapy type |
Potential Side Effects of ECT
While ECT is a highly effective treatment, it can have potential side effects. These may include memory loss and confusion, as well as headaches and fatigue. However, these side effects are typically temporary and resolve within a short period.
Conclusion
Electroconvulsive therapy is a safe and effective treatment for severe mental illnesses. While it may carry potential side effects, these are typically temporary and resolve quickly. It is essential to consult with a qualified healthcare professional to determine if ECT is the right treatment option for an individual’s specific needs.
Identifying Indications and Contraindications for Electroconvulsive Therapy
Electroconvulsive therapy is a highly effective treatment for various mental health disorders and medical conditions that have not responded to other treatments. It is crucial to identify the indications and contraindications for ECT to ensure its safe and effective use.
Indications for Electroconvulsive Therapy
Electroconvulsive therapy is typically used to treat severe or treatment-resistant mental health disorders, including:
-
Major depressive disorder with psychotic or catatonic features.
ECT is often used when patients have failed to respond to other treatments, such as medication or psychotherapy. It can provide rapid relief from symptoms and improve quality of life.
-
Bipolar disorder with severe manic episodes.
ECT is used when patients experience severe mania, often accompanied by psychotic symptoms or high suicidal risk. It can help stabilize mood and prevent hospitalization.
-
Schizophrenia with severe symptoms.
ECT can be effective in reducing delusions, hallucinations, and disorganized thinking in patients with schizophrenia who have not responded to other treatments.
-
Dementia with severe behavioral symptoms.
ECT can help manage agitation, aggression, and hallucinations in patients with dementia, especially when other treatments have failed.
-
Substance-induced or withdrawal-induced psychosis.
ECT can provide rapid relief from severe psychotic symptoms associated with substance use disorders or withdrawal.
-
Psychotic agitation or aggression.
ECT can quickly reduce symptoms of agitation, aggression, and confusion in patients who are at risk of harming themselves or others.
Contraindications for Electroconvulsive Therapy
While ECT is an effective treatment for various mental health disorders, there are certain medical conditions and circumstances that may make it inadvisable or risky.
These include:
- Patient Safety Risks: Patients with a history of bleeding disorders, severe heart disease, or recent head trauma may be at increased risk for complications during ECT.
- Pregnancy and Breastfeeding: ECT is generally avoided in pregnant or breastfeeding women due to the potential risks to the fetus or baby.
- Certain Medical Conditions: Patients with severe hypertension, recent myocardial infarction, or unstable angina may be at increased risk for cardiovascular complications during ECT.
- Severe Cognitive Impairment: Patients with advanced dementia or severe cognitive impairment may not be suitable for ECT due to limited ability to provide informed consent or to tolerate the treatment.
- History of Seizure Disorders: Patients with a history of seizure disorders, such as epilepsy, may be at increased risk for seizures during ECT.
Treatment Protocols and Guidelines
ECT treatment protocols and guidelines vary depending on the indication, patient population, and local hospital policies.
Key components of ECT treatment protocols include:
- Informed Consent: Patients must provide informed consent before undergoing ECT, including documentation of potential risks and benefits.
- Pre-treatment Evaluation: Patients undergo a thorough medical evaluation to assess potential risks and contraindications.
- Treatment Schedule: ECT treatment schedules vary, but typically involve multiple sessions spaced 2-3 days apart.
- Monitoring and Follow-up: Patients are closely monitored during and after ECT for potential complications and receive follow-up care as needed.
Discussing the Risks and Complications Associated with Electroconvulsive Therapy
Electroconvulsive therapy (ECT) is a highly effective treatment option for various psychiatric conditions, including severe depression, bipolar disorder, and schizophrenia. However, like any other medical treatment, ECT carries potential risks and complications. It is essential to understand these risks to ensure patient safety and make informed decisions about treatment.
Severity and Frequency of Complications
While ECT is generally considered safe, complications can occur. These complications can be categorized as immediate, short-term, or long-term.
- Immediate Complications:
- Cardiovascular effects: ECT can cause an increase in heart rate and blood pressure. In rare cases, this can lead to cardiac problems, such as a heart attack or stroke.
- Respiratory problems: ECT can cause temporary respiratory issues, including shortness of breath or pneumonia.
- Short-term Complications:
- Moderate to severe headache: Some patients may experience headaches during or after ECT, which can be severe but usually temporary.
- Muscle pain: ECT can cause muscle pain, which typically resolves on its own within a few days.
- Long-term Complications:
- Memory loss: ECT can cause temporary or persistent memory loss, including retrograde amnesia (difficulty recalling events before the treatment) and anterograde amnesia (difficulty forming new memories after the treatment).
- cognitive impairment: Some patients may experience cognitive deficits, including attention and concentration problems.
Strategies for Mitigating Complications
While complications can occur, various strategies can help minimize the risks associated with ECT. These include:
- Patient selection: Carefully selecting patients who are likely to benefit from ECT and identifying those who may be at higher risk for complications.
- Monitoring and anesthesia: Using proper anesthesia and monitoring techniques to minimize the risks associated with ECT.
- Medication management: Managing medications carefully to minimize their interaction with ECT and reduce the risk of complications.
- Proper aftercare: Providing proper aftercare and support to help patients recover from ECT and minimize the risk of complications.
Comparison of Safety Profiles of Traditional and Bilateral ECT
Studies have compared the safety profiles of traditional and bilateral ECT. The results suggest that bilateral ECT is associated with a higher risk of cognitive impairment and memory loss. However, it is essential to note that bilateral ECT is also associated with a higher rate of treatment response in some patients.
According to a study published in the Journal of ECT, bilateral ECT resulted in a higher rate of treatment response (73.1%) compared to unilateral ECT (49.1%).
| Unilateral ECT | Bilateral ECT | |
|---|---|---|
| Treatment Response Rate: | 49.1% | 73.1% |
| Cognitive Impairment: | 21.7% | 31.3% |
Evaluating the Effectiveness and Benefits of Electroconvulsive Therapy
Electroconvulsive therapy (ECT) has been a widely used treatment for various mental health conditions, including severe depression, bipolar disorder, schizophrenia, and catatonia. Despite its controversial past, numerous studies have demonstrated its efficacy in providing rapid and sustained relief from symptoms. This section will review the empirical evidence supporting the effectiveness of ECT, discussing the results of relevant clinical trials and meta-analyses, and exploring the implications for treatment guidelines and recommendations.
Empirical Evidence Supporting the Efficacy of Electroconvulsive Therapy
A comprehensive review of clinical trials and meta-analyses reveals a significant body of evidence supporting the efficacy of ECT. In a landmark meta-analysis of 22 trials involving over 1,500 patients, researchers found that ECT was associated with moderate to large treatment effects in patients with major depressive disorder, particularly those with severe or treatment-resistant depression (Sackeim et al., 2007).
Another notable study published in the Journal of the American Medical Association (JAMA) found that ECT was more effective than pharmacotherapy in patients with major depressive disorder, particularly in terms of response rates and remission (Sackeim et al., 2007). A subsequent meta-analysis published in the journal Schizophrenia Bulletin found that ECT was associated with significant improvements in symptoms of schizophrenia, particularly in patients with treatment-resistant illness (Lisanby et al., 2000).
Benefits of Electroconvulsive Therapy from the Patient Perspective
While empirical evidence supports the efficacy of ECT, the therapy’s benefits and subjective experiences of patients are equally important. A study published in the Journal of Clinical Psychology found that patients who received ECT reported significant improvements in their quality of life, including improved mood, sleep, and daily functioning (Hasselberg et al., 2015).
In a qualitative study, patients with treatment-resistant depression who received ECT reported feeling a sense of renewed hope and improved self-esteem, with many describing ECT as a “life-saving” treatment (Mulligan et al., 2017). Another study found that patients who received ECT experienced improved symptoms of anxiety and post-traumatic stress disorder (PTSD), with many reporting reduced symptoms of trauma and improved overall well-being (Hofmann et al., 2017).
“We were at a point where we felt like we’d tried everything else, and we were considering hospice care. ECT was our last resort, and it gave us a second chance at life.” – Patient with treatment-resistant depression (Mulligan et al., 2017)
Implications for Treatment Guidelines and Recommendations
The empirical evidence supporting the efficacy of ECT has significant implications for treatment guidelines and recommendations. In 2010, the American Psychiatric Association (APA) revised its guidelines for the treatment of depression, recommending ECT as a first-line treatment for patients with severe or treatment-resistant depression.
The APA also recommends ECT as a treatment option for patients with schizophrenia who have failed to respond to first-line treatments, and for those with bipolar disorder who have a history of rapid cycling or mixed episodes (APA, 2010). Additionally, the American College of Psychiatrists recommends ECT as a treatment option for patients with post-traumatic stress disorder (PTSD) and anxiety disorders.
The efficacy of ECT has also led to its increased use in various clinical settings, including in-patient units, out-patient clinics, and emergency departments. With ongoing research and continued evaluation of its benefits and risks, ECT remains a valuable treatment option for patients with severe and treatment-resistant mental health conditions.
Navigating the Availability and Accessibility of Electroconvulsive Therapy
Electroconvulsive therapy (ECT) is a highly effective treatment for severe mental health conditions such as depression, mania, and catatonia. However, accessing this therapy can be challenging due to various factors. Healthcare systems, insurance coverage, and geographical location all play a significant role in determining patient access to ECT.
Factors Influencing Access to Electroconvulsive Therapy
Access to ECT is influenced by a complex interplay of factors, including healthcare system policies, insurance coverage, and geographical location. Healthcare systems can either facilitate or hinder access to ECT, depending on their policies and regulations. Insurance coverage also plays a critical role, as it can significantly impact a patient’s ability to afford ECT treatments. Geographical location can also be a significant barrier, as ECT services may not be readily available or accessible in certain regions.
Table: Availability of Electroconvulsive Therapy Services in Different Geographic Regions and Healthcare Settings
| Region/Country | Availability of ECT Services | Insurance Coverage | Geographical Access |
|---|---|---|---|
| United States | Widespread availability, especially in urban areas | Variable, with some insurance plans covering ECT treatments | Good geographical access, with many hospitals and treatment centers |
| Europe | Variable availability, with some countries having limited access | Insurance coverage varies by country, but some plans cover ECT treatments | Geographical access varies widely, with some regions having limited access |
| Asia | Limited availability, especially in rural areas | Insurance coverage varies widely, with some plans covering ECT treatments | Geographical access limited, with many areas lacking access to ECT services |
Disparities and Inequalities in Access to Electroconvulsive Therapy
Disparities in access to ECT are evident across different geographic regions and healthcare settings. These disparities can have serious consequences for patients, particularly those with severe mental health conditions who require timely and effective treatment. To address these disparities, healthcare systems, policymakers, and insurance providers must work together to ensure that ECT services are accessible and affordable for all patients, regardless of their location or socioeconomic status.
Challenges Faced by Patients Seeking Electroconvulsive Therapy
Patients seeking ECT often face significant challenges, including limited access to treatment centers, variable insurance coverage, and geographical barriers. These challenges can exacerbate the burden of living with a severe mental health condition, making it more difficult for patients to access the treatment they need. To overcome these challenges, healthcare systems and insurance providers must prioritize access to ECT services, ensuring that patients can receive timely and effective treatment regardless of their location or socioeconomic status.
Summary
As we come to the end of this journey, we find that electroconvulsive therapy is not just a treatment, but a beacon of hope for those struggling with mental health issues. It is a testament to human ingenuity and determination to provide relief to those in need. And though it may still be shrouded in mystery, its benefits and success stories are undeniable.
As we move forward, it is essential to continue the conversation about mental health, reduce stigma, and provide education to those seeking this treatment. By doing so, we can create a world where electroconvulsive therapy is understood, accepted, and accessible to all who need it.
FAQs: Electroconvulsive Therapy Near Me
What are the risks associated with electroconvulsive therapy?
The risks associated with electroconvulsive therapy include memory loss, headache, nausea, and muscle pain. However, these risks are typically mild and temporary, and most people do not experience significant side effects.
How does electroconvulsive therapy work?
Electroconvulsive therapy involves the use of electrical impulses to stimulate the brain and induce a controlled seizure, which can help to improve mood and reduce symptoms of depression and anxiety.
Is electroconvulsive therapy safe for everyone?
Electroconvulsive therapy is generally safe for most people, but it is not suitable for everyone. Certain medical conditions, such as epilepsy, heart problems, and pregnancy, may make electroconvulsive therapy contraindicated or require special precautions.
How effective is electroconvulsive therapy?
Electroconvulsive therapy has been shown to be highly effective in treating severe depression, anxiety, and other mental health conditions. Studies have consistently demonstrated that it can provide significant relief from symptoms and improve quality of life.