Keratoconus doctor near me is a crucial search for individuals struggling with this progressive eye condition, which affects the shape of the cornea and can lead to significant vision problems. In this comprehensive guide, we will delve into the world of keratoconus, exploring its causes, symptoms, diagnosis, and treatment options. Our aim is to empower you with the knowledge to navigate the journey to recovery and find the right specialist near you.
From understanding the definition and types of keratoconus to learning about the various treatment options, including corneal cross-linking and contact lenses, we will cover it all. We will also discuss the importance of early detection and the role of keratoconus specialists in managing this condition. Whether you are seeking information on how to detect keratoconus symptoms or exploring ways to cope with the emotional impact of living with this condition, we have got you covered.
Keratoconus Overview
Keratoconus is a progressive eye disease that affects the shape of the cornea, leading to distorted vision and potentially severe vision loss if left untreated. It occurs when the cornea, the clear dome-shaped surface at the front of the eye, bulges or thins, causing the eye to become irregularly shaped. This condition can be challenging to diagnose and may require a comprehensive eye exam to detect.
The symptoms of keratoconus can vary in severity and may include blurred vision, sensitivity to light, eye strain, and double vision. The condition can progress slowly, with the cornea becoming increasingly irregular and distorted over time. Early detection and treatment are essential to slow the progression of the disease and prevent further complications.
Types of Keratoconus
Keratoconus can be classified into three main types: congenital, acquired, and degenerative.
- Acquired Keratoconus: This is the most common type and usually develops in the teenage years or early adulthood. It is believed to be caused by a combination of genetic and environmental factors, such as excessive eye rubbing or eye allergies.
-
Acquired keratoconus has two subtypes:
- Progressive Keratoconus
- Posterior Keratoconus
Acquired keratoconus is further divided into two subtypes: progressive keratoconus and posterior keratoconus. Progressive keratoconus is characterized by a gradual thinning of the cornea and is often associated with a family history of the condition. Posterior keratoconus, on the other hand, affects the back of the cornea and can lead to severe vision loss if left untreated.
- Congenital Keratoconus: This rare type of keratoconus is present at birth and can be detected during a routine eye exam. It is often associated with other eye conditions, such as astigmatism and myopia.
- Degenerative Keratoconus: This type of keratoconus occurs in older adults and is often associated with other age-related eye conditions, such as cataracts and glaucoma.
Disease Progression and Complications
The progression of keratoconus can vary significantly from person to person. In some cases, the condition may progress slowly, while in others, it may progress rapidly. If left untreated, keratoconus can lead to severe complications, including vision loss, eye pain, and even corneal transplants.
Keratoconus can be further complicated by other eye conditions, such as:
- Corneal ectasia: a condition where the cornea becomes thin and irregular, leading to vision distortion and eye pain.
- Posterior keratoconus: a condition where the back of the cornea becomes irregular, leading to severe vision loss.
“Early detection and treatment of keratoconus are crucial to slowing the progression of the disease and preventing further complications.” – American Academy of Ophthalmology
Causes and Risk Factors of Keratoconus
Keratoconus is a complex eye disorder that has been associated with various potential genetic and environmental factors, which can contribute to its development. Understanding these factors can help individuals take preventative measures and alleviate symptoms.
Genetic Factors
Genetics play a significant role in the development of keratoconus. Research has shown that the condition can be inherited in an autosomal dominant pattern, meaning that a single copy of the mutated gene is enough to increase the risk of developing keratoconus. Individuals with a family history of keratoconus are more likely to develop the condition.
Genetic Associations
- The most common genetic association is with the CHST6 gene, which is responsible for encoding the protein necessary for maintaining the structure of the cornea.
- Other genes associated with keratoconus include PAX6, PITX3, and LOXL1.
- The genetic basis of keratoconus is not fully understood, and more research is needed to determine the underlying mechanisms.
Environmental Factors
In addition to genetic factors, several environmental factors have been linked to the development of keratoconus. These include:
Environmental Associations
- Allergies: Individuals with allergies, particularly those that affect the skin and eyes, are more likely to develop keratoconus.
- Ocular trauma: Physical damage to the cornea, such as in the aftermath of an accident, can lead to keratoconus.
- Hormonal imbalances: Hormonal fluctuations during pregnancy and puberty can increase the risk of developing keratoconus.
- Refractive error: Individuals with high myopia or hyperopia are more likely to develop keratoconus.
Hormonal Imbalances
Hormonal imbalances, particularly those affecting the growth and development of the cornea, can increase the risk of developing keratoconus. Hormones such as estrogen and testosterone play a crucial role in maintaining the structure of the cornea.
Hormonal fluctuations during pregnancy and puberty can lead to changes in the cornea, increasing the risk of keratoconus.
Allergies
Allergies, particularly those that affect the skin and eyes, can increase the risk of developing keratoconus. The immune system’s response to allergens can lead to inflammation and damage to the cornea.
Allergic Associations, Keratoconus doctor near me
- Atopic dermatitis: Individuals with a history of atopic dermatitis are more likely to develop keratoconus.
- Chronic rhinitis: Long-term allergies affecting the nose and throat can increase the risk of developing keratoconus.
- Conjunctivitis: Eye infections that lead to inflammation and damage to the cornea can increase the risk of keratoconus.
Ocular Trauma
Physical damage to the cornea, such as in the aftermath of an accident, can lead to keratoconus. This type of trauma can cause inflammation, scarring, and structural changes to the cornea, increasing the risk of developing keratoconus.
Ocular Trauma Associations
- Corneal laceration: Deep cuts to the cornea can lead to scarring and structural changes, increasing the risk of keratoconus.
- Blunt trauma: A blow to the eye can cause inflammation, scarring, and changes to the cornea, increasing the risk of keratoconus.
- Penetration injury: Pokes or stabs to the eye can lead to inflammation, scarring, and changes to the cornea, increasing the risk of keratoconus.
| Causes / Risk Factors | Associated Symptoms |
|---|---|
| Genetics | Eye discomfort, irregular vision, and sensitivity to light |
| Allergies | Itchy, watery eyes, redness, and swelling in the eyes and surrounding area |
| Ocular trauma | Pain, bleeding, and vision loss |
| Hormonal imbalances | Chronic eye irritation, vision distortion, and increased sensitivity to light |
Detecting and Diagnosing Keratoconus
Detecting keratoconus early is crucial to prevent further vision loss and ensure effective treatment. A comprehensive eye exam, which includes a self-examination and various diagnostic tests, plays an essential role in identifying keratoconus symptoms and confirming the diagnosis.
Step-by-Step Guide to Self-Examination for Keratoconus Symptoms
When conducting a self-examination for keratoconus symptoms, pay attention to the following aspects:
- Dryness and irritation in the eyes, possibly caused by thinning corneas
- A distorted, blurred, or irregular-shaped vision
- Discomfort or sensitivity to light, especially when wearing contact lenses or using digital devices
- Rapid vision deterioration or fluctuations in nearsightedness or astigmatism
- Movements of the iris (the colored part of the eye)
- Fatigue or strain while performing daily activities due to vision challenges
The symptoms may worsen over time if left undiagnosed or untreated, highlighting the importance of regular eye check-ups for those at risk.
Diagnostic Tests Used in Keratoconus Diagnosis
Ophthalmologists employ various diagnostic tests to confirm the diagnosis and rule out other eye conditions that may exhibit similar symptoms. These tests include:
* Visual Acuity Tests: Measure the sharpness of your vision to determine the severity of your condition and monitor any improvement or deterioration over time.
* Corneal Topography: Provides a detailed map of your cornea’s surface, revealing any irregularities, such as cone-shaped protrusions.
* Pachymetry: Measures the thickness of your cornea to determine the rate of thinning.
* Dilated Retinoscopy: Involves using special drops to dilate the pupils, followed by the use of a retinoscope to examine the retina and detect any abnormal curvature of light as it enters the eye.
* Computerized Imaging: Uses specialized software to produce detailed 3D images of the cornea, aiding in the assessment of cone shape and progression.
Comparing Diagnostic Methods Used by Eye Care Professionals
Each diagnostic test has its specific role in the comprehensive evaluation of keratoconus. While corneal topography is often considered the gold standard in identifying cone-shaped protrusions, visual acuity tests help monitor vision changes and assess the effectiveness of treatment.
In addition to these tests, eye care professionals may use other diagnostic tools, such as corneal tomography or optical coherence tomography (OCT), to examine the cornea and retinal layers in more detail.
A thorough diagnostic process enables ophthalmologists to accurately diagnose and develop a treatment plan tailored to the unique needs of each patient with keratoconus.
Treatment Options for Keratoconus
Keratoconus is a progressive eye disease that requires timely and effective treatment to prevent further vision loss. Fortunately, various treatment options are available to manage the condition, including corneal cross-linking, contact lenses, refractive surgery, and corneal transplant for advanced cases.
Corneal Cross-Linking (CXL)
This process slows down the progression of keratoconus and maintains the structure of the cornea. The procedure involves applying a riboflavin solution to the eyes and then exposing them to ultraviolet light. This treatment is particularly useful for patients with early to moderate keratoconus.
Soft and Rigid Gas Permeable Contact Lenses
Contact lenses can provide temporary relief from keratoconus-related vision issues. Soft gas permeable lenses are designed to be comfortable and flexible, while rigid gas permeable lenses are more durable and often preferred for advanced cases of keratoconus. They can be used as an alternative to CXL or in combination with other treatments to correct vision.
Refractive Surgery (LASIK/PRK)
Refractive surgery, such as LASIK (Laser-Assisted In Situ Keratomileusis) or PRK (Photorefractive Keratectomy), can be used to correct vision issues related to keratoconus. However, patients with advanced keratoconus may not be candidates for refractive surgery, as the procedure requires a stable corneal surface.
Corneal Transplant
For advanced cases of keratoconus, a corneal transplant may be necessary. This surgical procedure involves removing the diseased cornea and replacing it with a healthy one from a donor. A corneal transplant can help restore vision and prevent further vision loss.
According to the American Academy of Ophthalmology, corneal transplantation is a safe and effective procedure with a success rate of over 90%.
In addition to these treatment options, patients with keratoconus should work closely with their eye care providers to monitor the progression of the disease and adjust treatment plans as necessary. Early detection and treatment can significantly improve outcomes and prevent further vision loss.
Working with a Keratoconus Specialist
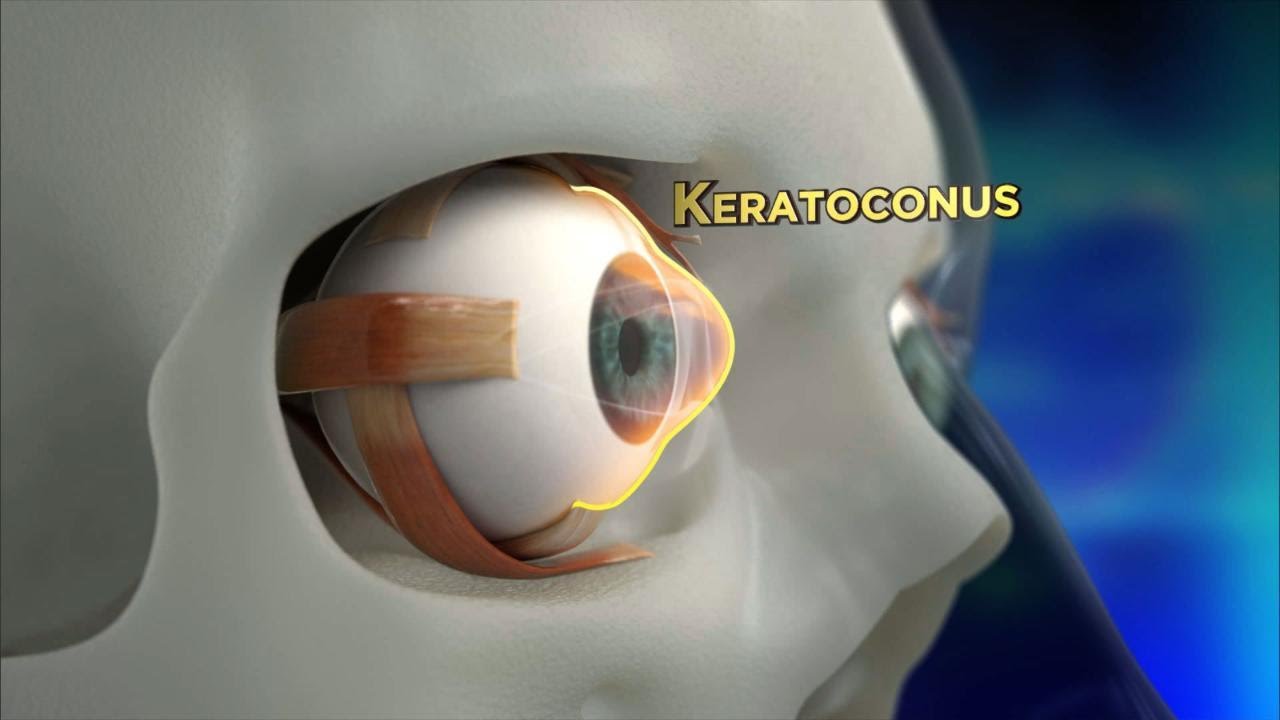
Working with a keratoconus specialist is crucial in effectively managing the condition. These dedicated professionals have extensive knowledge and experience in diagnosing and treating keratoconus. By consulting a keratoconus specialist, patients can receive personalized care and guidance throughout their treatment journey.
A good doctor-patient relationship is essential in managing keratoconus, as it enables open communication and trust. This rapport allows patients to feel comfortable sharing their concerns and questions, facilitating a more accurate diagnosis and effective treatment plan. Moreover, a good relationship with a keratoconus specialist helps patients stay engaged in their care, leading to better adherence to treatment recommendations.
Establishing a Good Doctor-Patient Relationship
Establishing a strong doctor-patient relationship is vital in managing keratoconus effectively. This relationship is built on trust, respect, and open communication. Patients should feel comfortable sharing their concerns, and their keratoconus specialist should be approachable and willing to address these concerns. By establishing a good relationship, patients can expect improved treatment outcomes and a better overall experience.
- Active listening: A keratoconus specialist should actively listen to patients’ concerns and respond in a compassionate and empathetic manner.
- Clear communication: Patients should receive clear and concise explanations of their diagnosis, treatment options, and expected outcomes.
- Personalized care: A keratoconus specialist should tailor their care approach to each patient’s unique needs and circumstances.
Ongoing Eye Care and Follow-up Appointments
Regular follow-up appointments and ongoing eye care are essential in preventing keratoconus progression. During these appointments, keratoconus specialists can monitor patients’ condition, make adjustments to their treatment plan as needed, and ensure patients are adhering to their treatment recommendations. By attending regular follow-up appointments, patients can expect to maintain optimal vision and prevent further complications.
Questions to Ask a Potential Keratoconus Specialist during a Consultation
When consulting a potential keratoconus specialist, patients should be prepared with a list of questions to discuss their treatment options and expectations. This enables patients to make informed decisions about their care and ensures they receive the best possible treatment for their keratoconus.
- What are the treatment options available for my keratoconus, and which one do you recommend?
- How will we monitor my condition, and what milestones can I expect to reach with treatment?
- How will we address any complications that may arise during treatment, and what contingency plans are in place?
- Can I receive regular follow-up appointments, and how often will we review my treatment plan?
Self-Care and Management Strategies
Taking care of your overall health and well-being is crucial in managing keratoconus. By following these self-care and management strategies, you can help prevent keratoconus-related complications and improve your quality of life.
Good Eye Hygiene
Proper eye hygiene is essential in maintaining the health of your eyes. To prevent eye infections and promote healing, follow these steps:
- Wash your hands thoroughly before touching your eyes.
- Remove your contact lenses before sleeping and disinfect them regularly.
- Clean and dry your eyelids daily to prevent the buildup of allergens and debris.
- Use artificial tears to lubricate and soothe your eyes, especially during dry or windy weather.
- Consult your doctor about the best cleaning and disinfecting solutions for your contact lenses.
Regular Exercise and Balanced Diet
Regular exercise and a balanced diet can help alleviate stress, promote overall health, and even slow the progression of keratoconus. Here are some tips:
- Exercise regularly, aiming for at least 30 minutes of moderate physical activity per day.
- Eat a balanced diet rich in fruits, vegetables, whole grains, and lean proteins.
- Avoid sugary or processed foods that can exacerbate inflammation and oxidative stress.
- Stay hydrated by drinking plenty of water throughout the day.
- Consider consulting a registered dietitian for personalized nutrition advice.
Stress Management and Relaxation Techniques
Keratoconus-related anxiety and stress can be overwhelming. Practice these relaxation techniques to manage stress and promote overall well-being:
- Meditation: Take a few minutes each day to sit comfortably, close your eyes, and focus on your breath.
- Deep breathing exercises: Inhale deeply through your nose, hold your breath for a few seconds, and exhale slowly through your mouth.
- Progressive muscle relaxation: Tense and then relax different muscle groups in your body, starting with your toes and moving up to your head.
- Yoga: Engage in gentle stretches and poses to reduce stress and improve flexibility.
- Journaling: Write down your thoughts and feelings to process and release emotions.
Stress-Reducing Exercises and Activities
In addition to relaxation techniques, engage in stress-reducing activities to manage keratoconus-related anxiety:
- Gentle stretching or yoga to improve flexibility and reduce stress.
- Listening to calming music or nature sounds to promote relaxation.
- Engaging in creative activities like painting, drawing, or writing to express emotions.
- Spending time in nature, such as walking or hiking, to reduce stress and promote well-being.
- Practicing gratitude by reflecting on the things you are thankful for each day.
Sample Menu for Keratoconus Patients
Here is a sample menu that includes nutrient-rich foods to help manage keratoconus:
| Foods | Benefits |
|---|---|
| Fatty fish (salmon, sardines, and mackerel) | Rich in omega-3 fatty acids to reduce inflammation. |
| Nuts and seeds (almonds, walnuts, and chia seeds) | High in antioxidants and healthy fats to promote eye health. |
| Leafy greens (spinach, kale, and collard greens) | Packed with vitamins A, C, and E to support eye health. |
| Berries (blueberries, strawberries, and raspberries) | Rich in antioxidants to reduce oxidative stress. |
Important Reminders
Remember to:
- Consult your doctor or a registered dietitian for personalized nutrition advice.
- Stay hydrated by drinking plenty of water throughout the day.
- Practice good eye hygiene and follow proper contact lens care.
- Manage stress through relaxation techniques and activities.
Coping with Keratoconus-Related Anxiety
Living with keratoconus can be physically and emotionally challenging, leading to anxiety, stress, and feelings of isolation. The emotional impact of keratoconus can be significant, affecting mental health and overall well-being. It’s essential to address keratoconus-related anxiety and seek support from family, friends, and support groups.
Emotional Impact of Keratoconus
The emotional impact of keratoconus can be intense, with patients experiencing feelings of anxiety, fear, and frustration. These emotions can stem from concerns about vision loss, the uncertainty of treatment outcomes, and the burden of managing a chronic condition. In severe cases, anxiety and depression can become debilitating, affecting daily life and relationships.
Seeking Support from Family, Friends, and Support Groups
Seeking support from loved ones, friends, and support groups is crucial in managing keratoconus-related anxiety. Sharing experiences and emotions with others who understand the challenges of keratoconus can help alleviate feelings of isolation and loneliness. Support groups, both online and in-person, provide a safe space to discuss concerns, receive guidance, and connect with others who face similar challenges.
Personal Stories and Testimonies
Many individuals have successfully managed keratoconus-related anxiety by seeking support and taking proactive steps to manage their condition. One patient, for example, found solace in joining a support group and learning about the latest treatment options. Another patient credits her therapist with helping her cope with anxiety and develop coping strategies.
Recommended Support Groups and Resources
Several organizations and resources offer support and guidance for individuals living with keratoconus. For example:
- National Keratoconus Foundation (NKF): A non-profit organization providing education, support, and advocacy for those affected by keratoconus.
- Keratoconus Support Group: An online community where individuals can connect, share experiences, and access resources.
- National Eye Institute (NEI): A leading source of information on eye health, including keratoconus, with resources for patients and healthcare professionals.
These organizations provide valuable resources, support, and guidance, helping individuals live with confidence, manage keratoconus-related anxiety, and maintain a high quality of life.
With the right support and resources, individuals with keratoconus can manage anxiety, take control of their condition, and live a fulfilling life.
Research and Emerging Treatments: Keratoconus Doctor Near Me
As research and technology continue to advance, new and innovative treatments for keratoconus are being developed. These emerging treatments aim to improve the management and treatment of keratoconus, providing patients with more effective and long-lasting solutions.
Ongoing Research and Clinical Trials
Ongoing research and clinical trials are focused on developing new treatments for keratoconus, including stem cell therapy, gene therapy, and immunotherapy. These studies aim to improve our understanding of the underlying causes of keratoconus and to identify new targets for treatment.
- Stem Cell Therapy: This approach involves using stem cells to regenerate damaged corneal tissue and restore the shape of the cornea.
- Gene Therapy: Researchers are exploring the use of gene therapy to modify the genes responsible for keratoconus, potentially preventing the progression of the disease.
- Immunotherapy: Immunotherapy aims to modulate the immune system’s response to keratoconus, reducing inflammation and damage to the cornea.
The results of these clinical trials are promising, and some have shown significant improvements in corneal shape and vision acuity. However, more research is needed to fully understand the potential benefits and limitations of these emerging treatments.
Regenerative Medicine
Regenerative medicine involves using stem cells, gene therapy, and other techniques to promote tissue regeneration and repair. In the context of keratoconus, regenerative medicine aims to regenerate damaged corneal tissue and restore the shape of the cornea.
Regenerative medicine has the potential to revolutionize the treatment of keratoconus, providing patients with more effective and long-lasting solutions.
Researchers are exploring various approaches to regenerative medicine for keratoconus, including:
- Stem Cell Therapy: As mentioned earlier, stem cell therapy involves using stem cells to regenerate damaged corneal tissue.
- Gene Therapy: Gene therapy aims to modify the genes responsible for keratoconus, potentially preventing the progression of the disease.
- Cellular therapies: Cellular therapies, such as mesenchymal stem cell therapy, have shown promise in promoting corneal regeneration and improving vision acuity.
Novel Contact Lens Designs and Technologies
Researchers are developing novel contact lens designs and technologies that can help manage keratoconus. These emerging technologies aim to improve the comfort, vision, and safety of contact lens wear for patients with keratoconus.
- Daily disposable contact lenses: Daily disposable contact lenses are designed for daily use and then discarded. They can provide a convenient and hygienic option for patients with keratoconus.
- Soft contact lenses: Soft contact lenses are designed to be more comfortable and breathable, reducing irritation and inflammation associated with keratoconus.
- Hybrid contact lenses: Hybrid contact lenses combine the comfort of soft lenses with the clarity of rigid lenses, providing excellent vision and comfort for patients with keratoconus.
These emerging treatments hold great promise for improving the management and treatment of keratoconus. However, more research is needed to fully understand their potential benefits and limitations.
Potential Benefits and Limitations
The potential benefits of emerging treatments for keratoconus include:
- Improved vision acuity and quality
- Reduced inflammation and damage to the cornea
- Increased comfort and convenience for patients
However, these treatments also have potential limitations, including:
- High costs associated with treatment
- Risk of complications and adverse reactions
- Limited availability and accessibility
As researchers continue to explore new treatments and technologies for keratoconus, it is essential to carefully evaluate the benefits and limitations of each approach and to prioritize patient safety and well-being.
Outcome Summary
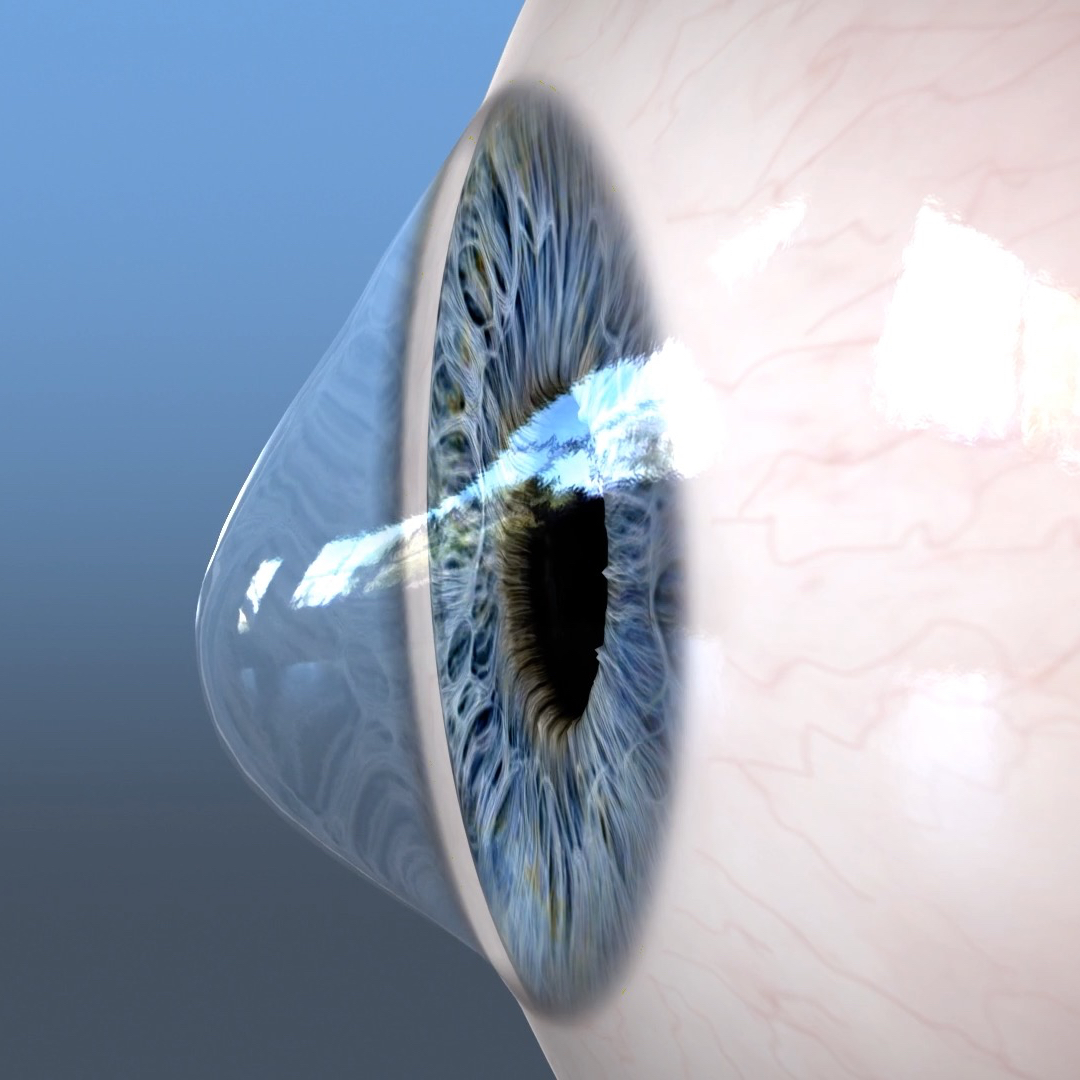
In conclusion, finding the right keratoconus specialist near you is a vital step in managing this condition. With the knowledge and resources provided in this guide, you are well-equipped to take control of your eye health and work towards a clearer, more confident vision. Remember, early detection and treatment are key to preventing further complications, and with the right care, you can say goodbye to keratoconus-related vision problems for good.
Helpful Answers
Q: What is keratoconus, and how is it diagnosed?
Keratoconus is a progressive eye condition that affects the shape of the cornea, leading to significant vision problems. It is typically diagnosed through a comprehensive eye exam, including visual acuity tests, corneal topography, and pachymetry.
Q: What are the treatment options for keratoconus?
The treatment options for keratoconus include corneal cross-linking, contact lenses (soft and rigid gas permeable), and refractive surgery. In advanced cases, corneal transplant may be necessary.
Q: How can I maintain good eye hygiene and prevent keratoconus-related complications?
Maintaining good eye hygiene is essential in preventing keratoconus-related complications. This includes washing your hands regularly, avoiding rubbing your eyes, and getting regular eye exams.