With oral maxillofacial surgeon near me at the forefront, this article explores the essential role of maxillofacial surgeons in dental care, their unique qualifications, and the importance of patient education. From defining the scope of practice to emerging trends in practice management, we’ll delve into the intricacies of maxillofacial care and provide valuable insights for patients seeking reliable maxillofacial surgeons near them.
Oral maxillofacial surgeons are specialized dentists who have undergone extensive training to manage a wide range of conditions affecting the mouth, face, and jaws. Unlike general dentists, they possess the expertise and skills to perform complex surgeries, including bone grafting, dental implant placement, and tissue reconstruction.
Defining the Role of an Oral Maxillofacial Surgeon
Oral maxillofacial surgeons are specialized dental professionals who possess advanced training and expertise in complex surgical procedures of the mouth, teeth, and facial structures. They possess the unique blend of dental and surgical knowledge to address multifaceted cases including those involving oral health, facial trauma, and cosmetic surgery. The role of an oral maxillofacial surgeon is distinct from that of a general dentist, necessitating a comprehensive understanding of both dental and anatomic principles.
The essential distinctions between the scope of practice of an oral maxillofacial surgeon and a general dentist lie in the nature and extent of the training, as well as the type of procedures they are qualified to perform. Oral maxillofacial surgeons typically undergo an additional 4-6 years of specialized education and training after dental school, encompassing a broad range of surgical specialties. This advanced training enables them to perform intricate surgical procedures that a general dentist would typically not attempt.
Examples of common procedures performed by oral maxillofacial surgeons that would be unsuitable for general dentists to attempt include:
Complex Facial Trauma Management
Oral maxillofacial surgeons are uniquely qualified to manage complex facial trauma cases, which often involve multiple fractures and soft tissue injuries. These cases necessitate a deep understanding of both anatomic and biomechanical principles to ensure proper alignment and healing of the affected structures. For instance, they may be called upon to repair fractures of the facial bones, restore the integrity of the maxillary sinus, or repair lacerations and soft tissue defects. Their expertise in managing these complex cases enables them to restore optimal function, aesthetics, and quality of life for patients.
Orthognathic Surgery and Dental Implantology
Oral maxillofacial surgeons are skilled in performing orthognathic (corrective jaw) surgery, which aims to restore the proper alignment and function of the jaw, teeth, and facial structures. They also possess advanced knowledge and expertise in dental implantology, enabling them to provide a comprehensive range of implant-related services, including the placement and restoration of dental implants. This combination of skills allows them to offer patients a full spectrum of treatment options for restoring optimal oral function and aesthetics.
Head and Neck Cancer Treatment and Reconstruction
Oral maxillofacial surgeons often play a critical role in the diagnosis and treatment of head and neck cancers. They work closely with other specialists to develop treatment plans that involve surgery, radiation, or chemotherapy. In some instances, they may also perform reconstructive surgery to repair defects, restore oral function, and enhance aesthetics.
Key Areas of Specialization, Oral maxillofacial surgeon near me
Oral maxillofacial surgeons possess expertise in three distinct areas of specialization:
- Complex Facial Trauma and Orthognathic Surgery
- Dental Implantology and Restorative Dentistry
- Head and Neck Cancer Treatment and Reconstruction
- Urban population density often results in higher concentrations of specialized facilities and services, including oral maxillofacial surgeons. This trend can lead to improved access for urban residents with complex maxillofacial conditions.
- However, urbanization can also result in the concentration of high-stakes cases in urban centers, straining the capacity of these facilities to meet demand. This, in turn, can create disparities in access to quality care between urban and rural populations.
- For instance, the location of vital structures such as the facial nerve, blood vessels, and salivary glands must be carefully considered during surgical planning to minimize the risk of injury and ensure optimal outcomes.
- Additionally, the use of advanced imaging technologies, such as computed tomography (CT) scans and magnetic resonance imaging (MRI), can facilitate more accurate diagnoses and help the surgeon plan the optimal approach for each case.
- Surgical management of dental implants, including implant placement, bone grafting, and restoration.
- Orthognathic surgery, including corrective jaw surgery for conditions such as obstructive sleep apnea, TMJ disorders, and malocclusion.
- Facial trauma management, including emergency surgery for facial fractures, lacerations, and other injuries.
- Cancer treatment and reconstruction, including excision of oral cancers, skin cancers, and lymph nodes, as well as reconstruction of facial tissues.
- Advantages of Hospital or Ambulatory Center Settings:
- Increased flexibility to offer specialized care
- Access to advanced equipment and technology
- Greater opportunities for multidisciplinary collaboration
- Improved ability to manage complex patient cases
- Considerations for Office-Based Models:
- Space constraints and limited resources
- Limitations in offering specialized care
- Potential compromises on patient comfort and continuity
- Enhance accuracy and precision in treatment planning
- Streamline communication between surgeons, lab technicians, and prosthetists
- Automate administrative tasks, reducing workload and improving productivity
- Enable more effective patient education and informed consent
- Patient outcomes
- Practice operations and efficiency
- Financial performance
- Continuing education and professional development
The oral maxillofacial surgeon’s advanced training and expertise in managing complex facial trauma cases and orthognathic surgery enable them to restore optimal function, aesthetics, and quality of life for patients.
Oral maxillofacial surgeons possess advanced knowledge and expertise in dental implantology, enabling them to provide a comprehensive range of implant-related services, including the placement and restoration of dental implants.
Oral maxillofacial surgeons work closely with other specialists to develop treatment plans that involve surgery, radiation, or chemotherapy and may also perform reconstructive surgery to repair defects, restore oral function, and enhance aesthetics.
Factors Influencing the Location of an Oral Maxillofacial Surgeon
Oral maxillofacial surgeons require a unique combination of surgical skills and knowledge of the head and neck region to effectively diagnose and treat complex maxillofacial conditions. The location of an oral maxillofacial surgeon’s practice can significantly impact access to quality care for patients with these conditions.
The topography of the maxillofacial region presents several challenges for surgical access and planning. This is particularly evident in situations where anatomically complex cases require intricate manipulation of the facial bones, nerves, and other vital structures. A well-equipped and experienced oral maxillofacial surgeon is, therefore, better placed to manage such cases more efficiently in an office environment.
Urbanization and Access to Quality Dental Care
Urbanization has been linked to an increased demand for specialized dental services, including oral and maxillofacial surgery. However, this trend has also led to concerns regarding unequal access to quality care in underserved or rural areas.
Urbanization has also led to changes in lifestyle, diet, and overall health habits, which can contribute to an increased incidence of complex maxillofacial conditions, including facial injuries, tumors, and orthognathic deformities. In this context, rural residents may face longer travel times and financial burdens associated with seeking specialized care in urban areas.
The oral maxillofacial surgeon must adapt treatment strategies to address these challenges. For instance, they may employ minimally invasive techniques or make use of advanced imaging technologies to facilitate more accurate diagnoses and improve treatment outcomes.
The adaptation of treatment strategies for anatomically challenging or rare conditions requires a deep understanding of the patient’s unique situation and the ability to think creatively. It also necessitates the utilization of cutting-edge technologies, including 3D printing and computer-aided design, to enhance surgical precision and optimize patient outcomes.
Maxillofacial Region Topography
The complex topography of the maxillofacial region presents challenges for surgical access and planning. In particular, anatomically complex cases may require intricate manipulation of the facial bones, nerves, and other vital structures.
Oral maxillofacial surgeons must possess a deep understanding of the complex anatomy of the maxillofacial region, as well as a range of surgical skills and techniques. They must also be adept at adapting treatment strategies to accommodate patients with anatomically challenging or rare conditions, using the most advanced technologies and techniques available.
In the context of anatomically complex cases, oral maxillofacial surgeons must balance the need for precision and delicacy with the need to address the patient’s specific needs and circumstances. This requires a high level of technical skill, as well as strong communication and interpersonal skills, to ensure that the patient understands the planned treatment and can provide informed consent.
Identifying the Credentials and Qualifications of an Oral Maxillofacial Surgeon: Oral Maxillofacial Surgeon Near Me
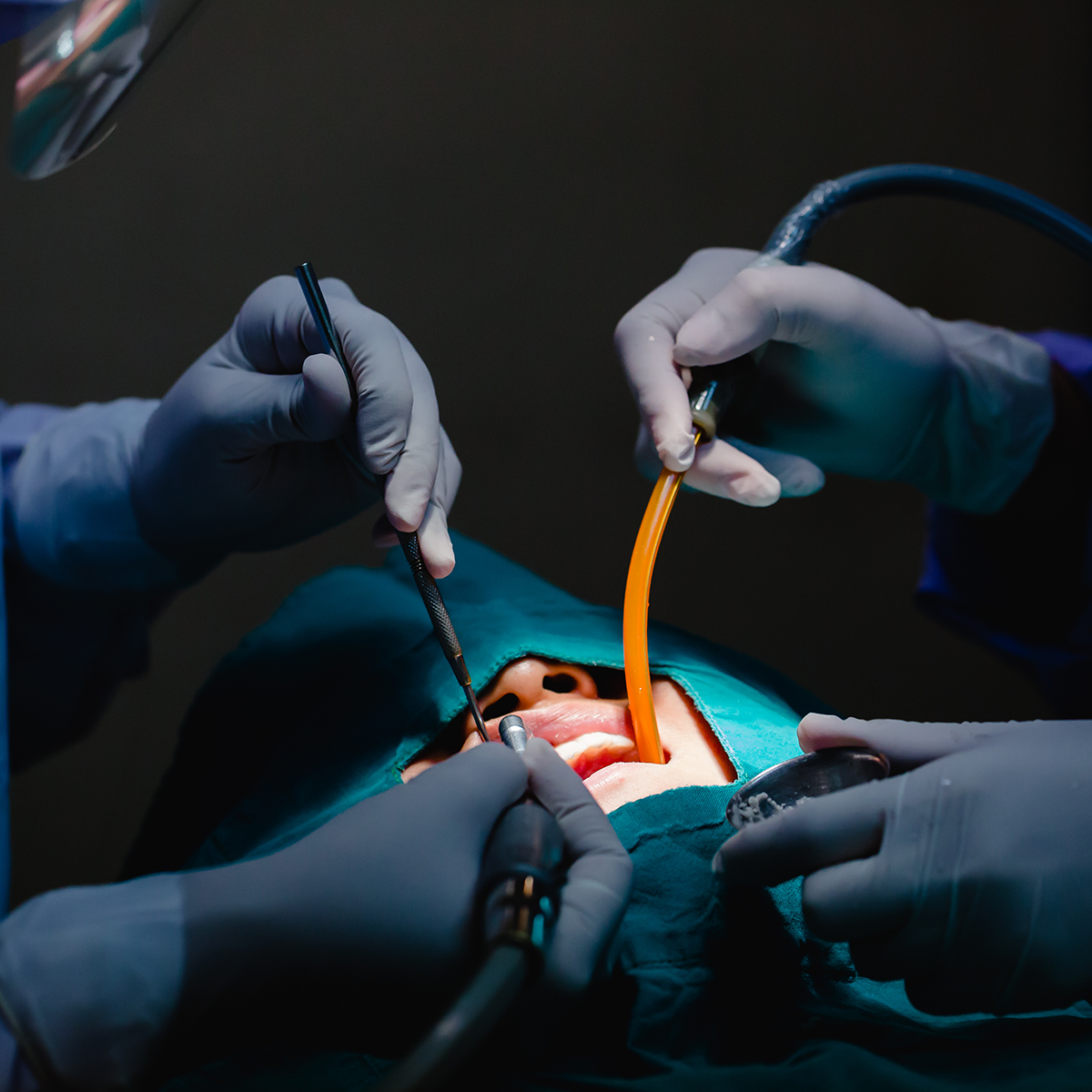
An oral maxillofacial surgeon is a specialized dentist who has undergone extensive education, training, and experience in the diagnosis, surgical treatment, and management of disorders and injuries affecting the mouth, jaws, and facial structures. To become a board-certified oral maxillofacial surgeon, one must possess a strong foundation in both dental and medical sciences.
Typical Educational Background and Formal Training Requirements
To become an oral maxillofacial surgeon, an individual must first earn a Doctoral degree in Dentistry (DDS or DMD) from an accredited dental program. This typically requires four years of graduate-level education and a comprehensive education in dental surgery, anatomy, physiology, biochemistry, and pharmacology. Following dental school, the aspiring oral maxillofacial surgeon must then complete a minimum of four to six years of advanced training through a residency program in oral and maxillofacial surgery. This residency program provides hands-on experience in surgical procedures, including orthognathic surgery, dental implantology, and facial trauma management.
Clinical Experience and Board Certification
In addition to formal training, oral maxillofacial surgeons must also gain extensive clinical experience by working under the supervision of experienced practitioners. After completing their residency program, they must pass a certification examination administered by the American Board of Oral and Maxillofacial Surgery (ABOMS). Board certification is a voluntary process, but it signifies a professional’s commitment to staying up-to-date with the latest research, techniques, and technologies in the field.
Overcoming Significant Challenges or Obstacles
Notable oral maxillofacial surgeons have overcome significant challenges to achieve their goals. Dr. William R. Lawson, Jr., a renowned oral and maxillofacial surgeon, has worked extensively with facial trauma patients and has developed innovative surgical techniques to improve patient outcomes. Another example is Dr. David A. Mitchell, who has made significant contributions to the field of orthognathic surgery, developing techniques to improve the accuracy and predictability of surgical corrections.
Types of Cases or Patients
An oral maxillofacial surgeon is the best choice for evaluation and treatment of a wide range of cases, including:
Surgical Expertise
Oral maxillofacial surgeons possess a broad range of surgical skills, including:
| Surgical Skills | Description |
|---|---|
| General anesthesia and sedation | Administering medications to induce and maintain a state of deep relaxation or unconsciousness. |
| Implant placement | Inserting dental implants into the jaw to support artificial teeth. |
| Craniofacial surgery | Possibly correcting birth defects, injuries, or other conditions that affect the skull and facial bones. |
Oral maxillofacial surgeons often work closely with other healthcare professionals to provide comprehensive care, ensuring the best possible outcomes for patients.
Emerging Trends in Oral Maxillofacial Surgery Practice Management
The management of an oral maxillofacial surgery clinic has evolved significantly over the years, adopting modern technologies and best practices to enhance efficiency and patient care. As the field continues to advance, oral maxillofacial surgeons must stay updated with the latest trends and innovations affecting their practice. This includes adopting new models of care delivery, leveraging cutting-edge technologies, and implementing data-driven strategies to optimize patient outcomes and business performance.
Traditional Office-Based Models vs. Hospital or Ambulatory Centers
The choice of practice setting has a considerable impact on an oral maxillofacial surgeon’s workflow and patient care. Traditional office-based models offer convenience and familiarity but often limit the range of services that can be offered due to space and resource constraints. In contrast, hospital or ambulatory center settings provide greater flexibility and opportunities for specialized care, but may compromise on patient comfort and continuity of care.
Traditionally, office-based models were the norm for oral maxillofacial surgery practices. These settings allowed surgeons to manage a wide array of procedures, from routine extractions to complex reconstructive surgeries. However, the limitations of office-based models became increasingly apparent as the scope of care expanded and patient needs became more complex. Hospitals and ambulatory centers have stepped in to fill this gap, offering specialized facilities and resources to support a broader range of procedures.
The shift towards hospital or ambulatory center settings has been driven by the growing demand for complex oral and maxillofacial surgical procedures, such as orthognathic surgery and craniofacial reconstruction. These procedures require sophisticated equipment, specialized staff, and controlled environments, which are more readily available in hospital or ambulatory settings.
The Impact of Dental Implantology Software on Efficiency and Effectiveness
Advances in dental implantology software have significantly enhanced the workflow of oral maxillofacial surgeons, streamlining procedures, improving accuracy, and enabling greater efficiency. These software solutions have the potential to transform clinical decision-making, automate administrative tasks, and optimize surgical outcomes.
Dental implantology software combines advanced diagnostic imaging, sophisticated treatment planning algorithms, and real-time patient data to enable more accurate and confident clinical decision-making. This software can:
The Strategic Importance of Data-Driven Quality Assessment
Data-driven quality assessment is critical to the effective management of an oral maxillofacial surgery clinic. By leveraging data analytics and quality metrics, surgeons can continually evaluate and improve patient care, optimize operational efficiency, and enhance the overall quality of the practice.
The American Association of Oral and Maxillofacial Surgeons (AAOMS) recommends that oral maxillofacial surgeons use data analytics to assess and improve quality in four critical areas:
End of Discussion
In conclusion, oral maxillofacial surgeons play a vital role in providing specialized care for patients with maxillofacial conditions. By understanding their qualifications, credentials, and the importance of patient education, patients can make informed decisions when seeking maxillofacial care. With emerging trends in practice management, it’s essential for oral maxillofacial surgeons to adapt to new technologies and workflows to deliver efficient and effective care to their patients.
Questions Often Asked
What is the difference between an oral maxillofacial surgeon and a general dentist?
Oral maxillofacial surgeons are specialized dentists who undergo extensive training to perform complex surgeries, such as bone grafting, dental implant placement, and tissue reconstruction. In contrast, general dentists provide routine dental care, such as check-ups, cleanings, and fillings.
Can an oral maxillofacial surgeon perform dental implant placement?
Yes, oral maxillofacial surgeons are trained to perform dental implant placement, including bone grafting and tissue reconstruction, to ensure optimal results for patients.
What is the educational background required to become an oral maxillofacial surgeon?
Oral maxillofacial surgeons typically complete a bachelor’s degree, followed by four years of dental school, and then an additional 4-6 years of surgical training through a hospital-based residency program.